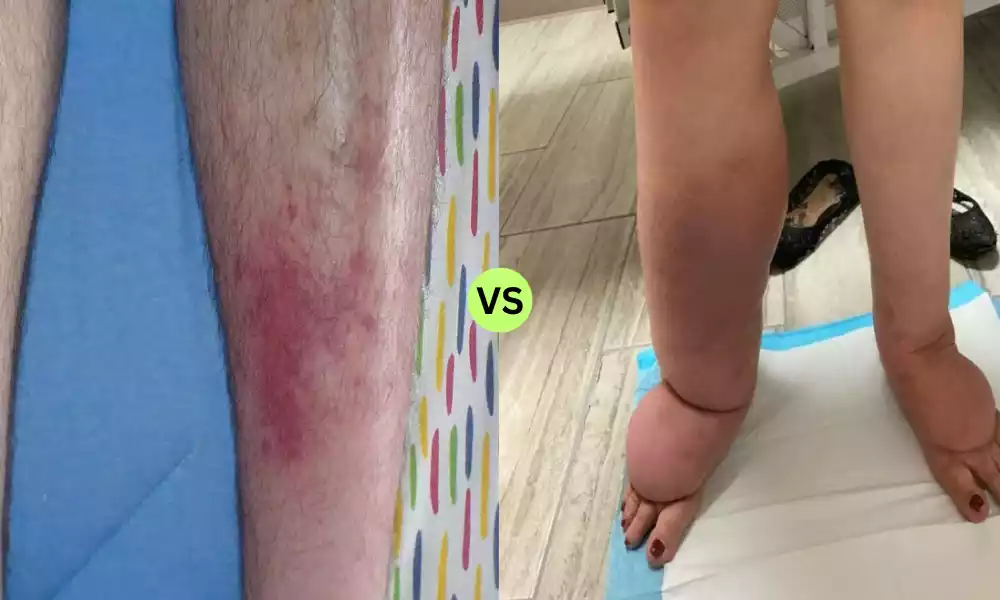
Cellulitis and Lymphedema: Cellulitis is an acute bacterial infection of the skin and subcutaneous tissue characterized by redness, warmth, swelling, and tenderness, often accompanied by fever. It typically arises after skin breaches, such as cuts or insect bites, allow bacteria to enter the deeper layers of the skin. Lymphedema, on the other hand, is a chronic condition resulting from the accumulation of lymph fluid in tissues, leading to swelling, typically in the arms or legs. It may arise due to impaired lymphatic system function or after surgical removal of lymph nodes, as seen in cancer treatments.
Both conditions require careful management, with cellulitis necessitating antibiotic treatment and lymphedema requiring interventions like compression therapy and manual lymph drainage.
Definition of Cellulitis
Cellulitis is a bacterial infection that affects the skin and its underlying soft tissues. Typically caused by streptococci and staphylococci bacteria, it manifests as a red, swollen, warm, and often painful area on the skin. These bacteria gain entry through breaks in the skin, such as cuts, insect bites, or surgical wounds. If untreated, cellulitis can progress and lead to serious complications, including the spread of the infection to the bloodstream.
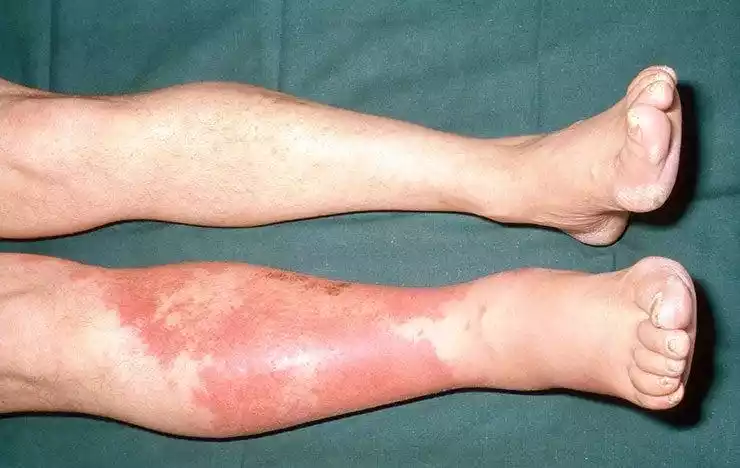
It’s typically managed with antibiotics, and early treatment is crucial to prevent severe outcomes. Proper wound care and hygiene can help in preventing the onset of this condition.
Causes and Symptoms of Cellulitis
Causes of Cellulitis
- Bacterial Infection: The primary cause of cellulitis is a bacterial infection. The most common bacteria responsible for cellulitis are:
- Streptococcus species (often Group A Streptococcus)
- Staphylococcus aureus (including Methicillin-resistant Staphylococcus aureus or MRSA in some cases)
- Breaks in the Skin: Bacteria, often present on the skin’s surface, can enter through:
- Cuts or wounds
- Surgical incisions
- Insect bites or stings
- Ulcers (such as venous or diabetic ulcers)
- Athlete’s foot or eczema (these conditions can cause skin cracks which allow bacteria to enter)
- Other Factors: Certain conditions or situations can increase the risk of developing cellulitis:
- Lymphedema (swelling due to the buildup of lymph)
- Chronic skin conditions (like eczema or psoriasis)
- Fungal infections
- Intravenous drug use
- Previous episodes of cellulitis
Symptoms of Cellulitis
- Skin Changes:
- Redness: The affected area becomes red.
- Swelling: The skin appears swollen or puffy.
- Warmth: The infected area is warm to the touch.
- Tenderness: The area is sensitive and may be painful to touch.
- Expansion: The red or swollen area can expand in size if not treated promptly.
- Pain: There’s usually pain or tenderness in the affected area.
- Systemic Symptoms: These can indicate that the infection is spreading or becoming severe:
- Fever and chills
- Feeling generally unwell or fatigued
- Swollen lymph nodes near the affected area
- Blisters or Pus: In some cases, blisters may form on the skin or the area may ooze clear fluid or pus.
- Skin Tightness: The skin may feel tight due to the swelling.
- Discoloration: As the cellulitis progresses or starts to heal, the skin might turn blueish or dark in color.
It’s crucial to recognize the symptoms of cellulitis early and seek medical attention, as untreated cellulitis can lead to more severe complications or spread rapidly.
Definition of Lymphedema
Lymphedema is a chronic condition characterized by the swelling of certain parts of the body, resulting from the accumulation of lymph fluid. This buildup occurs when there’s an impairment or disruption in the lymphatic system, often due to the removal or damage of lymph nodes from surgery, radiation treatments, or certain infections. The swelling can lead to pain, a feeling of heaviness, and a restricted range of motion in the affected area.
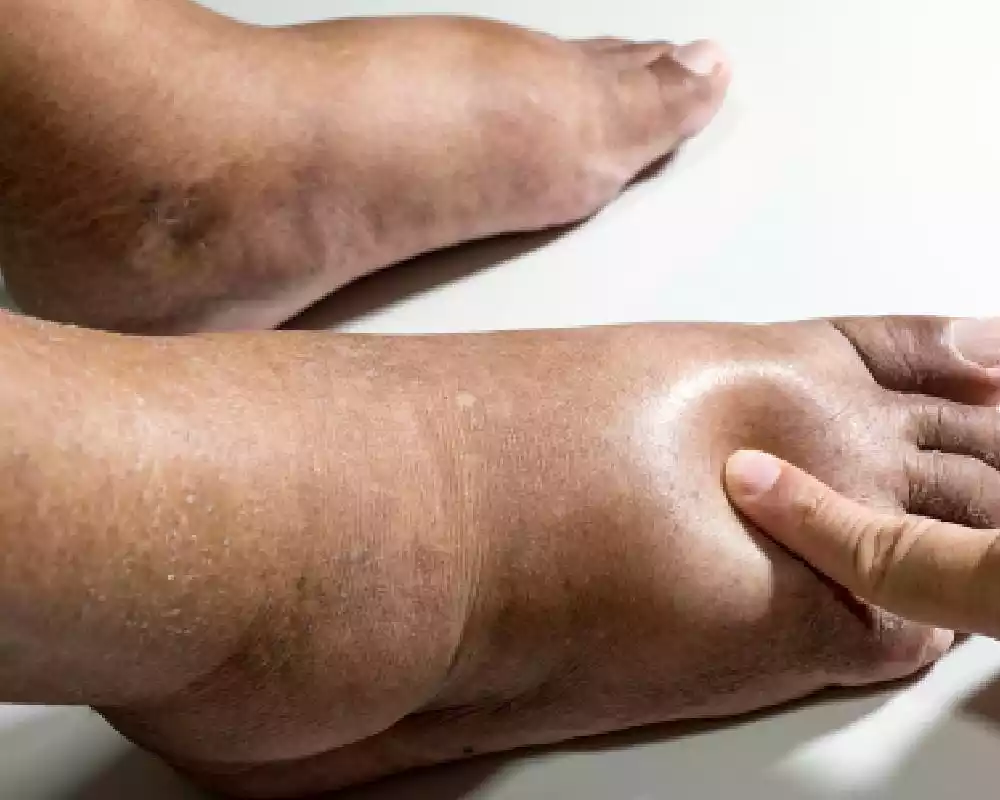
While there’s no cure for lymphedema, various treatments, including compression garments, massage, and exercises, can help manage and reduce the symptoms. It’s crucial for individuals with or at risk of lymphedema to avoid infections and injuries to the affected area, as these can exacerbate the condition.
Causes and Symptoms of Lymphedema
Causes of Lymphedema
Lymphedema results from damage to or a malfunction of the lymphatic system. The causes can be categorized into:
- Primary Lymphedema: This is a result of a congenital abnormality of the lymphatic system. It includes:
- Congenital lymphedema: Present at birth or develops by age two.
- Lymphedema praecox (Meige’s disease): It often starts during puberty.
- Lymphedema tarda: Begins after age 35.
- Secondary Lymphedema: This type arises from an external cause. It includes:
- Surgical procedures: Especially surgeries where lymph nodes are removed, as in breast cancer surgeries.
- Radiation therapy: Can damage or scar the lymph nodes or vessels.
- Infections: Parasitic infections or bacterial infections in the lymph nodes.
- Cancer: Tumors can block parts of the lymphatic system.
- Trauma or injury: Especially severe tissue injuries or burns.
- Chronic venous insufficiency: Long-term problems with the flow of blood in the veins can increase the risk of lymphedema.
- Inflammatory conditions: Conditions like rheumatoid arthritis or eczema.
- Cardiovascular diseases: Conditions that affect the veins of the legs.
Symptoms of Lymphedema
- Swelling: This is the hallmark symptom of lymphedema. A limb or other areas of the body (like the head, neck, or genitals) may appear swollen or puffy.
- Feeling of Heaviness or Tightness: The affected area may feel full or heavy.
- Restricted Range of Motion: Swelling may limit the movement of the affected limb.
- Aching or Discomfort: The affected area may be uncomfortable or even painful.
- Recurring Infections: The area can become prone to bacterial or fungal infections.
- Hardening and Thickening of the Skin (Fibrosis): Over time, the skin in the affected area can become hard and thick.
- Indentation: When pressed, the skin may retain an indentation, a condition called pitting.
- Fatigue: The increased weight and strain from the swelling can lead to tiredness.
Early detection and treatment of lymphedema are vital. While it’s a chronic condition, managing it effectively can help in reducing symptoms and preventing complications.
Comparison table of Cellulitis and Lymphedema
Below is the comparison table of cellulitis and lymphedema:
| Criteria | Cellulitis | Lymphedema |
|---|---|---|
| Definition | An acute, spreading bacterial infection of the skin and the tissues just beneath the skin surface. | A chronic condition characterized by the swelling of certain parts of the body due to the accumulation of lymph fluid. |
| Cause | Bacterial infection, often from Streptococcus or Staphylococcus, entering through breaks in the skin. | Blockage or damage to the lymphatic system, either congenital (primary) or due to external factors like surgery, radiation, etc. (secondary). |
| Appearance | Red, swollen, warm area on the skin. | Persistent swelling or puffiness, often in an arm or leg, but can be elsewhere. |
| Symptoms | – Redness
– Warmth – Swelling – Pain or tenderness – Fever and chills |
– Swelling in part or whole limb/area
– Heaviness or tightness – Restricted range of motion – Aching or discomfort – Skin changes (thickening, hardening) |
| Duration | Acute, but can recur. | Chronic and progressive. |
| Common Locations | Often on the lower legs but can occur anywhere. | Commonly affects arms or legs but can impact other body parts. |
| Treatment | Antibiotics (oral or intravenous) for bacterial infection. | – Compression therapy
– Manual lymphatic drainage – Exercises – Skin care |
| Complications | – Abscess formation
– Sepsis – Spread to deeper tissues |
– Infections like cellulitis
– Lymphangitis – Skin changes and fibrosis – Lymphangiosarcoma (rare) |
| Prevention/Management | – Good hygiene
– Prompt treatment of cuts and wounds |
– Regular limb exercises
– Skin care and infection prevention – Wearing compression garments |
This table provides a concise comparison of the two conditions. It’s important to understand that while there are distinct differences between cellulitis and lymphedema, one can be a complication of the other, as lymphedema increases the risk of cellulitis in the affected limb.
Risk Factors for Cellulitis
The development of cellulitis can be influenced by various risk factors that increase an individual’s susceptibility to the condition. Here are some notable risk factors for cellulitis:
- Breaks in the Skin: Any breach in the skin’s protective barrier can allow bacteria to enter and cause an infection. This includes:
- Cuts, abrasions, or wounds
- Surgical incisions
- Insect bites or stings
- Ulcers (e.g., venous, diabetic, or pressure ulcers)
- Dry, flaking, or cracked skin from conditions such as eczema or athlete’s foot
- Weakened Immune System: People with a compromised immune system are at a higher risk. This can be due to:
- Conditions like HIV/AIDS or diabetes
- Medications like corticosteroids or chemotherapy
- Organ transplantation (due to immunosuppressive drugs)
- Lymphedema: Swelling due to a buildup of lymph fluid can make the skin more vulnerable to infections and cellulitis.
- Previous Episodes of Cellulitis: Having had cellulitis in the past increases the risk of developing it again.
- Intravenous Drug Use: Injecting drugs can introduce bacteria into the body, increasing the risk of cellulitis.
- Chronic Swelling or Edema: Chronic swelling, especially in the legs, can make the skin more prone to infection.
- Obesity: Excessive body weight can lead to problems like poor circulation and edema, which can increase the risk of skin infections.
- Age: Older adults may have more fragile skin and a less efficient immune system, putting them at greater risk.
- Peripheral Vascular Disease: Poor circulation from conditions that affect the blood vessels can lead to increased susceptibility.
- Chronic Skin Conditions: Conditions like eczema, psoriasis, or fungal infections can compromise the skin’s integrity and function as a protective barrier.
- History of Venous Insufficiency: Poor blood flow in the veins, especially of the legs, can lead to skin changes and increased risk of infection.
Recognizing and addressing these risk factors, when possible, can help in preventing cellulitis or reducing its recurrence. Regular skin care, maintaining good hygiene, managing underlying conditions, and promptly treating wounds can also play a significant role in prevention.
Risk Factors for Lymphedema
Lymphedema is a condition characterized by localized fluid retention and tissue swelling resulting from a compromised lymphatic system. Several risk factors can increase an individual’s chances of developing this condition:
- Surgery: Procedures that require the removal or damage of lymph nodes, such as mastectomy for breast cancer, are a significant risk factor for developing lymphedema.
- Radiation Treatment: Radiation therapy, especially for cancer, can damage or scar lymph nodes or vessels, leading to lymphedema.
- Cancer and Tumors: Cancer cells can block lymphatic vessels. For instance, a tumor growing near a lymph node or lymph vessel might enlarge enough to block the flow of the lymph fluid.
- Infections: Some infections, especially parasitic infections, can damage the lymph nodes or vessels. In regions where filariasis (a parasitic disease) is common, it’s a major cause of lymphedema.
- Trauma or Injury: Any injury to the lymph nodes or lymphatic vessels can potentially cause lymphedema.
- Chronic Venous Insufficiency: This condition is characterized by the veins not efficiently sending blood from the legs back to the heart. Over time, it can lead to increased pressure in the veins, which can damage the lymph vessels and contribute to lymphedema.
- Age: Older adults may have a slightly increased risk of developing lymphedema.
- Obesity: Excess body weight is a risk factor for developing lymphedema because of the added strain on the lymphatic system.
- Rheumatoid or Psoriatic Arthritis: Inflammatory conditions can affect the lymph nodes and contribute to lymphedema.
- Family History: Primary lymphedema (caused by developmental issues with the lymphatic system) can run in families, suggesting a genetic link.
- Previous Episodes of Cellulitis: Recurrent infections can damage the lymphatic system and increase the risk of lymphedema.
Recognizing these risk factors and taking preventive measures, especially after surgeries or treatments that affect the lymphatic system, can help reduce the chances of developing lymphedema. Early intervention and management are crucial for controlling the condition and preventing complications.
Diagnosis of Cellulitis and Lymphedema
Diagnosing both cellulitis and lymphedema often involves a clinical examination, patient history, and, in some cases, further diagnostic tests.
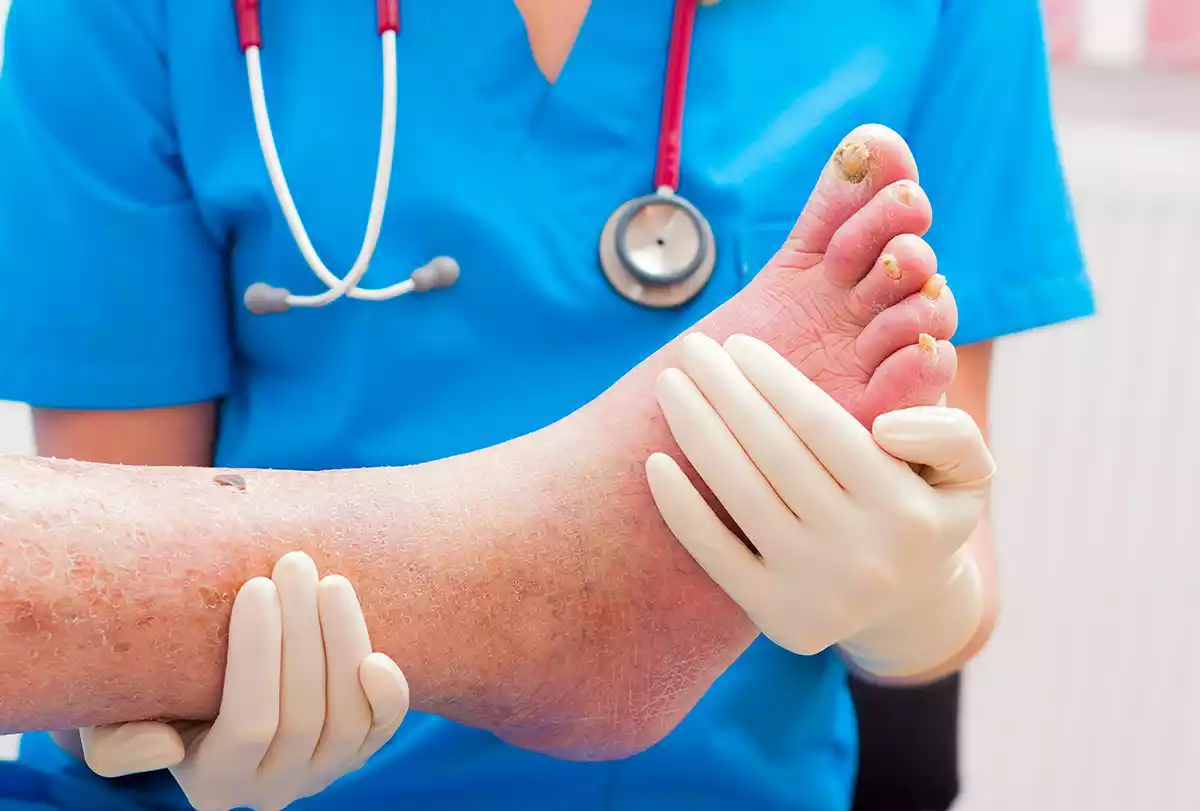
Here’s how each condition is typically diagnosed:
Diagnosis of Cellulitis:
- Clinical Examination: A physician will examine the affected area for signs of redness, warmth, swelling, and tenderness.
- Medical History: Information about recent injuries, surgeries, or other conditions that might predispose someone to skin infections will be collected.
- Blood Tests: While not always necessary, blood tests can be conducted to check for an elevated white blood cell count, which might indicate an infection.
- Culture: In some cases, especially if the infection doesn’t respond to initial treatment, a sample from the skin or from any draining fluid might be taken for lab testing to identify the specific bacteria causing the infection.
- Imaging: Rarely, if the physician suspects that the infection has spread deeper or if an abscess has formed, imaging studies like an MRI or ultrasound might be needed.
Diagnosis of Lymphedema:
- Clinical Examination: The physician will examine for swelling and other physical symptoms consistent with lymphedema. They’ll also assess the skin’s texture and thickness.
- Medical History: Information about any surgeries, treatments, infections, or injuries that could have affected the lymphatic system will be collected.
- Lymphoscintigraphy: This imaging test can visualize lymph flow. Radioactive dye is injected into the body, and special imaging cameras then track its movement through the lymphatic system.
- Doppler Ultrasound: This imaging method uses sound waves to produce images of the inside of the body. It can help differentiate between lymphedema and other causes of limb swelling, such as blood clots or venous insufficiency.
- MRI or CT Scan: In certain cases, these imaging methods can provide detailed images of the lymphatic system and help rule out other causes of swelling.
- Bioimpedance Spectroscopy: This non-invasive test measures the amount of fluid in the limb. It can detect increases in fluid even before visible swelling occurs.
- Volume Measurement: By submerging the limb in a water-filled tank or using a tape measure, healthcare providers can measure the volume and changes in volume of the affected limb.
- Stemmer’s Sign: This simple test involves pinching the skin on the base of the second toe or middle finger. If a skin fold cannot be easily lifted but rather remains thickened, it’s a positive Stemmer’s sign, often indicative of lymphedema.
An accurate diagnosis is crucial for both conditions. For cellulitis, prompt treatment is essential to prevent the spread of the infection. For lymphedema, early diagnosis and management can help in reducing symptoms and preventing complications.
Treatment Options for Cellulitis and Lymphedema
Both cellulitis and lymphedema require timely and appropriate management to prevent complications and improve outcomes. Here’s a breakdown of the treatment options for each:
Cellulitis Treatment Options
- Antibiotics: The primary treatment for cellulitis is antibiotics, which target the underlying bacterial infection.
- Oral antibiotics, like amoxicillin or cephalexin, are commonly prescribed for mild to moderate cases.
- Severe or rapidly progressing cases may require hospitalization and intravenous (IV) antibiotics.
- Pain Relief: Over-the-counter pain relievers, like acetaminophen or ibuprofen, can help reduce pain and fever.
- Rest and Elevation: If a limb is affected, elevating it can help reduce swelling.
- Moisturizing: Keeping the skin moisturized can prevent cracking and reduce the risk of recurrent infections.
- Treat the Underlying Cause: If cellulitis is recurrent or chronic, identifying and managing any predisposing conditions (like athlete’s foot) is crucial.
Lymphedema Treatment Options
The main goal of lymphedema treatment is to reduce swelling and control the pain. Treatment might involve:
- Compression: Wearing compression garments, such as stockings or sleeves, can promote the flow of the lymph fluid out of the affected limb.
- Manual Lymphatic Drainage (MLD): This is a type of massage that encourages the flow of lymph fluid out of the affected limb. It should be performed by trained therapists.
- Physical Therapy: Specific exercises can help improve lymph drainage.
- Pneumatic Compression: A device is used to inflate and deflate a sleeve that’s worn over the affected limb, helping to massage and move the fluid.
- Complete Decongestive Therapy (CDT): This multi-step therapy includes MLD, compression bandaging, skin care, and exercises.
- Skin Care: Regular skin care reduces the risk of skin infections, which can worsen lymphedema. This includes moisturizing the skin and addressing any minor cuts or breaks promptly.
- Surgery: For severe cases that don’t respond to other treatments, surgical procedures might be an option. These can include:
- Lymph node transfer: Moving healthy lymph nodes to the affected area.
- Lymphaticovenous anastomosis: Creating a bypass for the blocked lymphatic system.
- Liposuction: To remove excess fluid and tissue in advanced cases.
It’s essential to note that while cellulitis can be cured with appropriate treatment, lymphedema is a chronic condition. The goal of lymphedema treatment is to manage symptoms and prevent complications rather than achieving a complete cure. Regular follow-up and adherence to treatment are crucial for both conditions to optimize outcomes and prevent complications.
Preventive Measures
Preventing cellulitis and lymphedema, or managing their recurrence, requires adopting certain practices and measures. Here’s a look at the preventive steps for each condition:
Cellulitis Preventive Measures
- Skin Care:
- Keep skin clean and moisturized.
- Avoid drying out the skin, which can cause cracks and invite infections.
- Treat conditions that cause skin breaks, such as eczema, athlete’s foot, and fungal infections.
- Protect the Skin:
- Wear protective gear when engaging in activities that could lead to cuts or scrapes.
- Use insect repellent to avoid insect bites.
- Promptly Treat Wounds:
- Cleanse any cuts or wounds immediately and apply an antibiotic ointment.
- Cover the wound with a bandage and change dressings regularly.
- Inspect Feet Regularly: Especially for diabetics, checking for cracks, fungal infections, or wounds can prevent foot cellulitis.
- Manage Risk Factors: Control conditions like diabetes, and avoid intravenous drug use.
- Avoid Tight-Fitting Clothing: This can cause skin chafing and minor skin breaks.
Lymphedema Preventive Measures
For individuals at risk of developing lymphedema or for those already diagnosed with it:
- Avoid Infections:
- Practice good skin hygiene.
- Treat cuts or scratches promptly.
- Wear gloves for activities that might lead to hand or nail injuries.
- Avoid hot tubs, saunas, or very hot baths.
- Apply lotion to prevent skin from drying and cracking.
- Avoid Constricting Your Limb:
- Don’t carry heavy bags on a limb at risk.
- Avoid blood pressure readings on the affected limb.
- Be cautious with tight-fitting clothing or jewelry.
- Exercise Regularly: Gentle exercises can help lymph fluid circulate. It’s essential to consult with a physical therapist familiar with lymphedema.
- Protect Your Limb:
- Use a thimble when sewing.
- Wear protective footwear.
- Use sunscreen and insect repellent to reduce the risk of skin irritations and bites.
- Avoid Extreme Temperatures: Sudden temperature changes can affect lymph flow. This includes avoiding direct exposure to cold temperatures, which can be damaging, and protecting the skin from burns.
- Elevate the Affected Limb: When possible, especially if swelling is noticed.
- Compression Garments: Wear them as advised by a healthcare provider.
- Regular Medical Check-ups: Stay vigilant and seek advice if any changes or concerns arise.
It’s essential to recognize the individual’s specific risks and tailor preventive measures accordingly. For those at high risk or with a history of either condition, regular medical check-ups and early intervention can be crucial in preventing complications.
Conclusion
Cellulitis and lymphedema are both conditions that affect the skin and underlying tissues, albeit for different reasons. Cellulitis is a bacterial infection characterized by redness, warmth, swelling, and tenderness, often stemming from breaks in the skin. Immediate treatment with antibiotics is crucial to halt the spread of the infection. On the other hand, lymphedema is a chronic condition resulting from a compromised lymphatic system, leading to localized fluid retention and tissue swelling.
Its management focuses on controlling swelling, improving lymphatic flow, and preventing complications. While both conditions can present with limb swelling, their causes, treatment, and management strategies differ significantly. Proper diagnosis and prompt intervention are essential to optimize outcomes for both disorders.