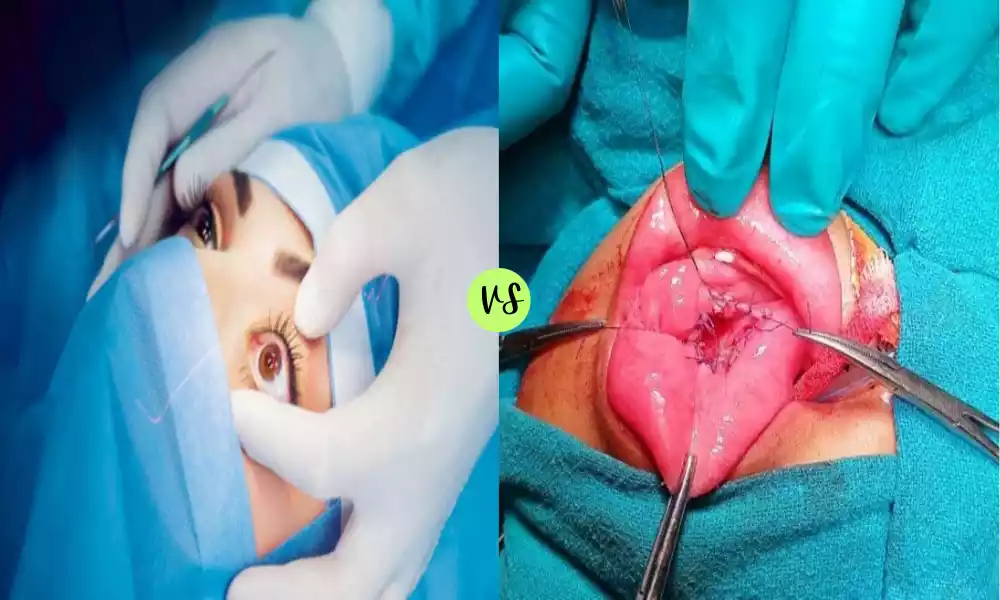
Enucleation and Marsupialization are surgical procedures primarily utilized in oral and maxillofacial surgery to address cysts and tumors. Enucleation refers to the complete surgical removal of a lesion, ensuring the preservation of surrounding tissues. This technique is particularly effective for well-defined, benign cysts or tumors.
Marsupialization involves opening the cyst, emptying its contents, and suturing its lining to form an open pouch, offering a less invasive approach especially suited for larger cysts or when vital structures might be compromised by complete removal. While both procedures aim to treat and manage oral lesions, the choice between them often depends on the specific clinical scenario and desired outcome.
What is Enucleation?
Enucleation is a surgical procedure that involves the complete removal of an organ or tissue structure, usually ensuring that the surrounding tissues are preserved. In ophthalmology, the term specifically refers to the removal of the entire eyeball while leaving the surrounding eye muscles and other orbital contents intact. This procedure is often performed due to malignant tumors, severe trauma, or end-stage eye diseases to prevent further complications or to alleviate pain.
Reasons for Enucleation
Enucleation, which refers to the surgical removal of the eyeball, is performed for various reasons. Here are some common indications for the procedure:
- Malignant Tumors:
- Retinoblastoma: A malignant tumor that primarily affects children and originates in the retina.
- Uveal Melanoma: A malignant tumor arising from the melanocytes of the uvea (iris, ciliary body, and choroid).
- End-stage Eye Diseases:
- End-stage Glaucoma: When intraocular pressure cannot be controlled, and the eye is blind and painful.
- End-stage Age-related Macular Degeneration (AMD): In situations where there’s no vision and significant pain.
- Trauma:
- Severe injuries causing irreparable damage to the eye.
- Situations where the injured eye might incite an immune response endangering the other healthy eye, a condition known as sympathetic ophthalmia.
- Infections:
- Severe, uncontrollable eye infections (endophthalmitis) that don’t respond to treatment and pose a risk of spreading.
- Painful Blind Eye:
- Eyes that have lost vision and cause continuous pain due to various diseases, where other treatments to alleviate pain are ineffective.
- Phthisis Bulbi:
- A shrunken, non-functional eye, which may be unsightly or painful.
- Cosmetic Reasons:
- In cases of eyes that are blind, disfigured, and unsightly due to various conditions or past surgeries.
- Congenital Anomalies:
- Some severe congenital or developmental malformations of the eye.
Enucleation is typically considered a last resort when other treatments have failed, are not viable, or when the eye poses a risk to the patient’s health or well-being. After enucleation, patients can often be fitted with an orbital implant and a custom prosthetic eye to achieve a cosmetically pleasing appearance.
The Process of Enucleation
Enucleation is a surgical procedure that involves the removal of the eyeball while preserving the surrounding structures, such as the eyelids, eye muscles, and orbital contents. Here’s a step-by-step breakdown of the process:
- Preoperative Evaluation:
- Medical History & Examination: Assessing the overall health of the patient, the reason for enucleation, and any potential complications.
- Imaging: In cases of tumors or trauma, imaging studies like CT or MRI might be conducted to evaluate the extent of the disease or injury.
- Discussion: Patients are informed about the procedure, potential risks, benefits, and alternatives. This aids in obtaining informed consent.
- Anesthesia:
- The procedure is typically performed under general anesthesia, ensuring the patient feels no pain and is unconscious throughout the procedure. In some cases, local anesthesia with sedation may be considered.
- Surgical Procedure:
- Incision: An incision is made in the conjunctiva (the clear tissue covering the white part of the eye).
- Muscle Dissection: The extraocular muscles (muscles responsible for eye movement) are carefully isolated and detached from the eyeball.
- Optic Nerve Severance: The optic nerve, which connects the eye to the brain, is identified and carefully severed.
- Removal: The eyeball is then delicately removed from the socket.
- Implant Placement: Often, an orbital implant is placed in the eye socket to replace the volume of the removed eyeball and maintain the structure of the socket. This implant can be made of various materials like silicone, porous polyethylene, or hydroxyapatite. The extraocular muscles might be attached to this implant to allow some movement.
- Closure: The conjunctival incision is then sutured closed, covering the orbital implant.
- Postoperative Care:
- Recovery Room: After the surgery, the patient is taken to a recovery room to wake up from anesthesia.
- Medication: Pain relievers and antibiotics may be prescribed to manage pain and prevent infections.
- Eye Covering: The eye may be bandaged for a day or more to protect the surgical site.
- Follow-up: Regular follow-up visits are scheduled to monitor healing and address any complications.
- Prosthetic Eye Fitting:
- After healing, which can take several weeks, a custom-made prosthetic eye (ocular prosthesis) can be created to fit over the operated area. This prosthesis mimics the appearance of a natural eye and improves cosmetic appearance. Periodic adjustments and replacements of the prosthesis might be needed over time.
- Rehabilitation and Counseling:
- Adjusting to life after enucleation can be challenging both physically and emotionally. Counseling and support groups can help patients cope with the psychological aspects of losing an eye.
It’s essential to understand that the decision to undergo enucleation is never taken lightly. It’s typically chosen when the benefits, such as eliminating pain or preventing the spread of a malignancy, outweigh the inherent risks and emotional impact of the procedure.
Recovery from Enucleation
Recovery from enucleation involves both physical healing of the surgical site and emotional adaptation to the loss of an eye. Here’s a breakdown of what one can expect during the recovery process:
Physical Recovery:
- Immediate Postoperative Period:
- Pain is a common complaint immediately after the surgery. Pain medications are prescribed to manage this.
- The eye socket will be covered with a pressure bandage to minimize swelling and bleeding. This is typically removed the day after surgery.
- First Week:
- Some swelling, bruising, and discharge can be expected.
- Antibiotic and sometimes steroid eye drops or ointments might be prescribed to prevent infection and reduce inflammation.
- Patients are advised to avoid activities that could strain the eyes, such as bending over, lifting heavy objects, or strenuous physical activity.
- First Month:
- Gradual reduction in swelling and bruising.
- Patients might notice a sensation as if the eye is still present, a phenomenon known as “phantom eye syndrome.”
- Sutures (if non-dissolvable) are removed during a follow-up visit.
- Six to Eight Weeks:
- By this time, the surgical site is typically well-healed.
- An ocularist can begin the process of fitting and creating a custom-made prosthetic eye.
- Long-term:
- Periodic check-ups with the ocularist may be needed for adjustments or replacements of the prosthetic eye.
- Regular follow-ups with the ophthalmologist or surgeon are crucial to monitor the health of the orbital socket and detect any potential issues early.
Emotional Recovery:
- Acceptance and Adaptation:
- Losing an eye can have a significant emotional and psychological impact. It’s normal for patients to go through a grieving process.
- Joining a support group or undergoing counseling can help in coping with the emotional aspects of the loss.
- Cosmetic Concerns:
- Once the prosthetic eye is fitted, most patients feel more confident about their appearance. The prosthetic eyes made today are very realistic and often difficult to distinguish from a natural eye.
- Adjustment to Monocular Vision:
- Losing vision in one eye can affect depth perception, particularly in near tasks. Over time, however, most patients adapt to using one eye for daily activities.
General Tips for Recovery:
- Eye Care: Keep the surgical site clean and dry. Use medications as prescribed.
- Activity: Avoid strenuous activities and protect the surgical site from potential trauma.
- Protection: Wear protective eyewear when necessary to shield the remaining eye, especially during sports or potentially hazardous activities.
- Stay Informed: Discuss any concerns or symptoms with the healthcare provider during the recovery process.
It’s essential for patients to have a good support system, including medical professionals, family, and friends, to aid in the physical and emotional aspects of recovery from enucleation.
What is Marsupialization?
Marsupialization is a surgical procedure used to treat cysts. During the procedure, the cyst is opened and its contents are removed. Instead of completely excising the cyst’s wall, a portion of it is sutured to the adjacent normal tissue, creating an open pouch. This allows the cyst to drain and gradually shrink over time. Marsupialization is commonly used for large cysts, particularly when they are located near vital structures, as it poses less risk to these structures than complete removal. This technique is frequently employed in the management of large jaw cysts or Bartholin’s cysts in gynecology.
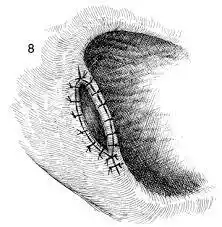
Why Marsupialization is Done?
Marsupialization is a surgical technique primarily employed to treat cystic lesions. The procedure involves creating an opening in the cyst so that its contents can drain and it can heal from the inside out. This technique is chosen over complete removal of the cyst in certain circumstances. Here are the reasons why marsupialization might be performed:
- Large Cysts:
- Marsupialization is often used for large cysts because it’s less invasive than completely excising the cyst. Removing a large cyst in its entirety could result in significant damage or alteration to surrounding tissues.
- Location near Vital Structures:
- If a cyst is located near crucial anatomical structures, marsupialization can minimize the risk of damaging these structures. For instance, in the case of large jaw cysts, there might be a risk of damaging nerves or tooth roots with complete excision.
- Recurrent Cysts:
- In situations where cysts have recurred after being treated with other methods, marsupialization might be chosen as an alternative approach to manage them.
- Bartholin’s Gland Cysts:
- Marsupialization is a common treatment for cysts or abscesses of the Bartholin’s gland in females. These glands are located on either side of the vaginal opening, and their cysts can be painful and recurrent.
- Pilonidal Cysts:
- For recurring or chronic pilonidal cysts located near the tailbone, marsupialization might be recommended, especially when there’s a sinus tract (a small tunnel in the skin).
- Ease of Procedure and Recovery:
- Marsupialization can be less invasive than other surgical procedures, potentially leading to shorter hospital stays and quicker recovery times.
- Preservation of Function:
- In some cases, marsupialization can help preserve the function of the tissue involved. For instance, in the case of an odontogenic keratocyst in the jaw, marsupialization can help in conserving the involved teeth and bone.
- Drainage and Relief:
- Marsupialization allows for continuous drainage of the cyst, which can alleviate symptoms like pain or pressure caused by the buildup of cystic fluid or other contents.
Marsupialization is not suitable for all types of cysts. The decision to use this technique depends on the type, location, and size of the cyst, the patient’s overall health, and the potential risks and benefits of the procedure.
The Process of Marsupialization
Marsupialization is a surgical procedure designed to treat cystic lesions by creating an opening, allowing for the continuous drainage of its contents and promoting healing from within. Here’s a step-by-step breakdown of the marsupialization process:
- Preoperative Evaluation:
- Medical History & Examination: A thorough assessment is conducted to evaluate the size, location, and characteristics of the cyst.
- Imaging: For some cysts, imaging studies like X-rays, ultrasound, CT, or MRI might be conducted to determine the cyst’s extent or its relationship with nearby structures.
- Discussion: Patients are informed about the procedure, its potential risks, benefits, and alternatives.
- Anesthesia:
- Depending on the cyst’s size and location, the procedure might be performed under local, regional, or general anesthesia.
- Surgical Procedure:
- Incision: A surgical incision is made on the cyst, usually at its most prominent or fluctuant part.
- Drainage: The contents of the cyst (fluid, pus, or other materials) are drained out.
- Debridement: Any necrotic or unhealthy tissue inside the cyst may be removed or debrided.
- Stitching the Edges: The edges of the cyst’s opening are sutured to the adjacent normal tissue, creating a pouch-like structure. This ensures the cyst remains open and continues to drain.
- Packing: In some cases, the opened cyst might be packed with a special dressing to promote drainage and healing from the inside. This packing may need to be changed periodically.
- Postoperative Care:
- Drainage Maintenance: Patients might be instructed to keep the area clean and ensure continuous drainage. This can involve cleaning the area with saline or other prescribed solutions.
- Medication: Pain relievers, antibiotics, or anti-inflammatory medications may be prescribed.
- Activity Limitation: Patients may be advised to avoid activities that might disrupt the surgical site, especially in the initial healing phase.
- Regular Follow-up: Follow-up visits will be scheduled to monitor healing, change dressings (if needed), and address any complications.
- Long-term Care:
- Observation: The marsupialized site needs to be observed for signs of recurrence, infections, or other complications.
- Hygiene: Maintaining cleanliness is crucial to prevent infections and promote optimal healing.
- Possible Further Treatment: If the cyst recurs or if marsupialization does not achieve the desired outcome, additional treatments or surgical procedures might be considered.
- Recovery:
- The recovery period depends on the cyst’s size, location, and the patient’s overall health. Generally, smaller cysts in accessible locations (like Bartholin’s cyst) might heal faster than larger cysts or those in more challenging locations.
It’s essential to follow postoperative instructions closely and communicate with healthcare providers about any concerns during the recovery process. While marsupialization is effective for many cysts, there’s still a risk of recurrence or complications, emphasizing the importance of regular follow-up and monitoring.
Recovery after Marsupialization
Recovery after marsupialization largely depends on the size, location, and type of cyst treated, as well as the patient’s overall health. Here’s an overview of the general recovery process following marsupialization:
- Immediate Postoperative Period:
- Pain and Discomfort: Patients may experience mild to moderate pain or discomfort in the surgical area. Over-the-counter painkillers or those prescribed by the doctor can help manage this.
- Drainage: It’s normal to notice some drainage from the marsupialized site. This drainage may decrease over time as the area heals.
- First Few Days:
- Wound Care: Keeping the surgical site clean is crucial. Patients might be instructed to clean the area with saline or another prescribed solution and to change dressings if they’ve been used.
- Activity Restrictions: Strenuous activities, heavy lifting, or other actions that might strain or disrupt the surgical site are typically discouraged.
- First Few Weeks:
- Healing: The marsupialized site will gradually heal. The pouch-like opening created during the surgery will typically shrink but may not close completely, allowing for continued drainage and preventing cyst recurrence.
- Follow-up Appointments: Regular check-ups with the surgeon or healthcare provider will be scheduled to monitor the healing process, remove sutures (if not absorbable), and address any concerns.
- Hygiene: Maintaining cleanliness around the surgical site continues to be essential to prevent infections and promote healing.
- Long-term Recovery:
- Observation: It’s essential to monitor the marsupialized area for any signs of complications, recurrence of the cyst, or other issues.
- Possible Further Treatment: If the cyst recurs or if marsupialization doesn’t achieve the desired result, additional treatments or procedures may be needed.
- Return to Activities: As the surgical site heals, patients can gradually return to their normal activities, always considering medical advice.
- Potential Complications:
- Infection: Signs of infection include increased redness, swelling, warmth, pus, or a foul odor from the surgical site. It’s essential to contact a healthcare provider if any of these signs are noticed.
- Bleeding: Some bleeding immediately after surgery is expected, but persistent or heavy bleeding should be reported to the doctor.
- Recurrence: There’s a chance the cyst could return, even after marsupialization. Regular monitoring and check-ups can help detect and address any recurrences early on.
- Emotional Recovery:
- Depending on the cyst’s location and significance to the patient, there might be emotional or psychological aspects to the recovery. It can be beneficial to discuss feelings or concerns with healthcare providers or consider joining support groups or counseling.
For the best recovery outcomes, it’s crucial to adhere to postoperative instructions, maintain regular follow-up appointments, and communicate any concerns or abnormal symptoms to the healthcare provider.
Comparison table of Enucleation and Marsupialization
Here’s a comparison table of Enucleation and Marsupialization:
| Feature/Aspect | Enucleation | Marsupialization |
|---|---|---|
| Definition | Complete removal of an organ or tissue structure. | Opening a cyst, removing its contents, and suturing a portion of its wall to create an open pouch. |
| Primary Use | Removal of the eyeball or oral/jaw cysts/tumors. | Treating large cysts, especially near vital structures. |
| Procedure Goal | Entirely remove the diseased or affected structure. | Reduce the cyst’s size and allow continuous drainage. |
| Tissue Removal | Entire tissue or organ is removed. | Only the contents of the cyst are removed, while a portion of its wall is left intact. |
| Surgical Closure | Wound is fully closed post-procedure. | Wound remains partially open to allow drainage. |
| Risk of Recurrence | Generally low, as the entire lesion is removed. | Higher, especially if used as the sole treatment. |
| Invasiveness | Can be more invasive, depending on the lesion’s size and location. | Typically less invasive, especially for larger cysts. |
| Recovery Time | May vary but could be longer due to the invasiveness of the procedure. | Generally quicker, though requires maintenance and monitoring of the drainage site. |
| Post-Op Maintenance | Regular wound care and monitoring for complications. | Continuous care for the drainage site and potential for further treatments if the cyst recurs. |
| Complications | Potential damage to adjacent structures. | Potential for infection or cyst recurrence. |
The choice between enucleation and marsupialization is often based on the specific clinical situation, the surgeon’s expertise, and the desired outcome. It’s essential to consult with a specialist when considering these procedures.
Similarities between Enucleation and Marsupialization
Enucleation and marsupialization are distinct surgical procedures with different primary objectives. However, they do share some similarities, primarily in the general context of surgical interventions. Here are some of the similarities between enucleation and marsupialization:
- Purpose of Treatment: Both procedures aim to treat specific medical conditions or diseases. Enucleation is primarily used for treating severe eye diseases or injuries, while marsupialization is used for certain cystic lesions.
- Surgical Intervention: Both are invasive procedures that require surgical intervention, often in a controlled environment like an operating room.
- Anesthesia: Both procedures might necessitate the use of anesthesia—local, regional, or general—depending on the specifics of the case and the patient’s overall health.
- Postoperative Care: After either surgery, there’s a period of recovery during which wound care, pain management, and follow-up visits with the surgeon or healthcare provider are essential. Both procedures come with specific postoperative care instructions that patients must follow to ensure optimal healing and outcomes.
- Risk of Complications: As with any surgery, both enucleation and marsupialization come with potential risks and complications, such as infection, bleeding, or adverse reactions to anesthesia.
- Hospital Stay: Depending on the specifics of the procedure and the patient’s overall health, both surgeries might require a hospital stay, either for observation or as part of the recovery process.
- Long-term Monitoring: After both procedures, long-term monitoring is crucial. For enucleation, this involves monitoring the health of the orbital socket and prosthetic eye fitting, if applicable. For marsupialization, this involves ensuring the cyst doesn’t recur and the marsupialized site heals well.
- Rehabilitation: Both procedures may involve a form of rehabilitation. Enucleation might require adapting to monocular vision and using a prosthetic eye, while marsupialization might involve learning wound care or managing drainage from the marsupialized site.
- Emotional Implications: Any surgical procedure can have emotional and psychological implications for the patient. Both enucleation, which involves the removal of an eye, and marsupialization, which might be associated with concerns about recurrence or appearance, can lead to emotional reactions that might benefit from counseling or support groups.
While these procedures share some common ground in the broad context of surgical interventions, it’s essential to understand that they address different medical conditions and have their own set of specific considerations, techniques, and outcomes.
Conclusion
Enucleation and marsupialization are surgical interventions designed to address specific medical conditions, with the former targeting severe eye diseases and the latter treating certain cystic lesions. Both procedures underscore the advancements in surgical techniques, offering patients the prospect of relief, improved quality of life, and better health outcomes.
While each surgery has its distinct methodologies, risks, and recovery processes, they share common grounds in terms of surgical preparation, the potential need for anesthesia, postoperative care, and the overarching goal of ensuring patient well-being. As with any surgical intervention, a thorough understanding by the patient, coupled with expert medical care, is paramount for optimal results.