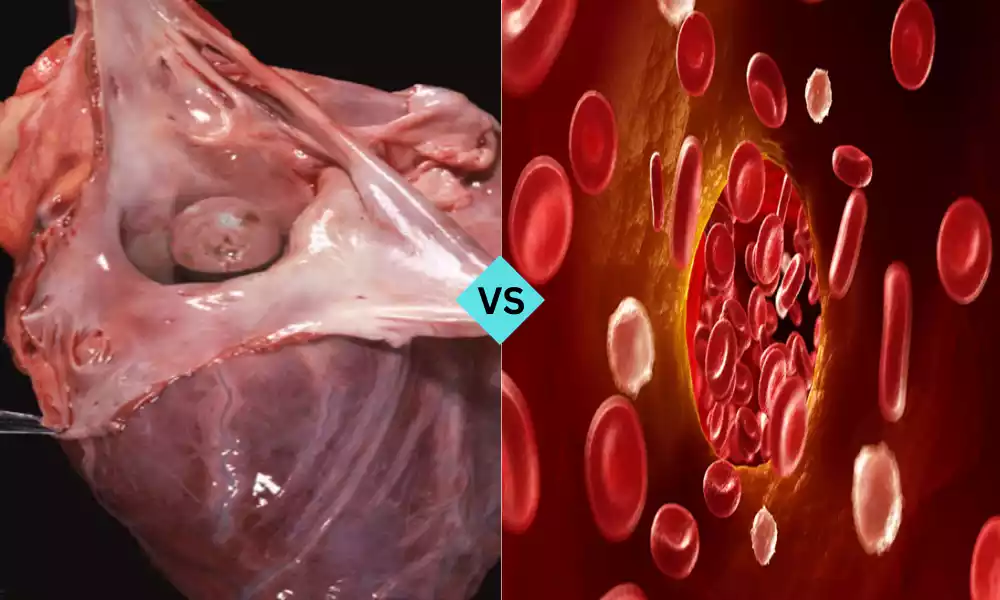
Myxoma and Thrombus are two cardiovascular conditions with distinct characteristics. Myxoma is a benign heart tumor, primarily found in the atria, causing symptoms related to cardiac and systemic issues. Thrombus, on the other hand, represents a blood clot that can develop in arteries or veins, leading to potentially severe conditions like heart attacks, strokes, or pulmonary embolism. Recognizing the disparities between these two conditions is crucial for prompt diagnosis and effective treatment.
What is Myxoma?
Myxoma is a rare type of cardiac tumor that originates in the heart. These tumors are typically benign, meaning they are non-cancerous. Myxomas are characterized by their gelatinous or mucous-like consistency and often grow within the atria of the heart, particularly the left atrium. While myxomas are relatively uncommon, they can cause a variety of symptoms and complications related to their size and location within the heart.

Types of Myxomas
- Atrial Myxoma: Atrial myxomas are the most common type. They originate within the atria of the heart, most often in the left atrium. Atrial myxomas can vary in size and can lead to a range of symptoms, including cardiovascular and systemic issues.
- Ventricular Myxoma: Ventricular myxomas are a rarer type. Unlike atrial myxomas, they develop within the ventricles of the heart. Although less common, they can still pose significant health risks and may require surgical intervention for removal.
Causes and Risk Factors
The exact cause of myxoma is not well understood. There are some risk factors and associations that have been identified:
- Familial Predisposition: There is evidence to suggest that some cases of myxoma may have a genetic component, with a family history of the condition.
- Carney Complex: This is a rare genetic disorder that can increase the risk of developing cardiac myxomas.
- Age and Gender: Myxomas are more commonly found in women and often occur in middle-aged individuals.
Symptoms of Myxoma
Myxomas can present with a wide range of symptoms, which can be attributed to their size, location, and the extent of interference with normal heart function. Common symptoms include:
- Cardiovascular Symptoms: These may include palpitations, shortness of breath, chest pain, and irregular heartbeats.
- Systemic Symptoms: Myxomas can release small particles into the bloodstream, leading to symptoms such as fever, weight loss, and joint pain.
- Neurological Symptoms: In some cases, patients may experience neurological symptoms, such as stroke, which can occur due to embolization of tumor particles.
- Physical Examination Findings: On examination, healthcare providers may detect a heart murmur, which can be indicative of a myxoma.
Diagnostic Procedures
Diagnosing myxoma typically involves a combination of clinical evaluation and medical imaging. Key diagnostic procedures include:
- Echocardiography: Echocardiograms are the primary imaging modality for diagnosing myxomas. This non-invasive test uses sound waves to create images of the heart, providing clear visualization of the tumor.
- Cardiac MRI: Magnetic resonance imaging (MRI) can provide more detailed information about the tumor’s location and characteristics.
- CT Scans: Computed tomography (CT) scans can be used to obtain cross-sectional images of the heart, aiding in the diagnosis of myxoma.
- Biopsy: In some cases, a biopsy of the tumor may be necessary to confirm the diagnosis. This is a less common procedure, as the risk of embolization during biopsy can be high.
Treatment Options for Myxoma
The treatment of myxoma typically involves surgical removal of the tumor. The main treatment options include:
- Cardiac Surgery: Open-heart surgery is often required to remove the tumor safely. During surgery, the heart is stopped, and a heart-lung machine is used to maintain oxygenation and circulation.
- Minimally Invasive Surgery: In some cases, minimally invasive approaches may be considered, particularly for smaller tumors. These procedures involve smaller incisions and reduced recovery times.
- Follow-Up: After surgery, patients will require regular follow-up to monitor their cardiac health and ensure there is no recurrence of the tumor.
Prognosis and Complications
The prognosis for myxoma is generally positive following successful surgical removal of the tumor. There can be complications and long-term effects, including:
- Recurrence: Although rare, myxomas can recur, necessitating further surgery.
- Embolic Events: The release of tumor particles into the bloodstream can lead to embolic events, such as strokes or blockages in other blood vessels.
- Heart Valve Dysfunction: Myxomas can interfere with heart valve function, leading to issues like regurgitation or stenosis.
What is Thrombus?
A thrombus is a blood clot that forms within a blood vessel, leading to the obstruction of blood flow. These clots can occur in arteries or veins, and they can have significant medical implications. Thrombosis is the process of thrombus formation and can lead to various health conditions, including heart attacks, strokes, deep vein thrombosis (DVT), and pulmonary embolism (PE). Understanding thrombus formation and its associated risks is essential for timely diagnosis and appropriate treatment.
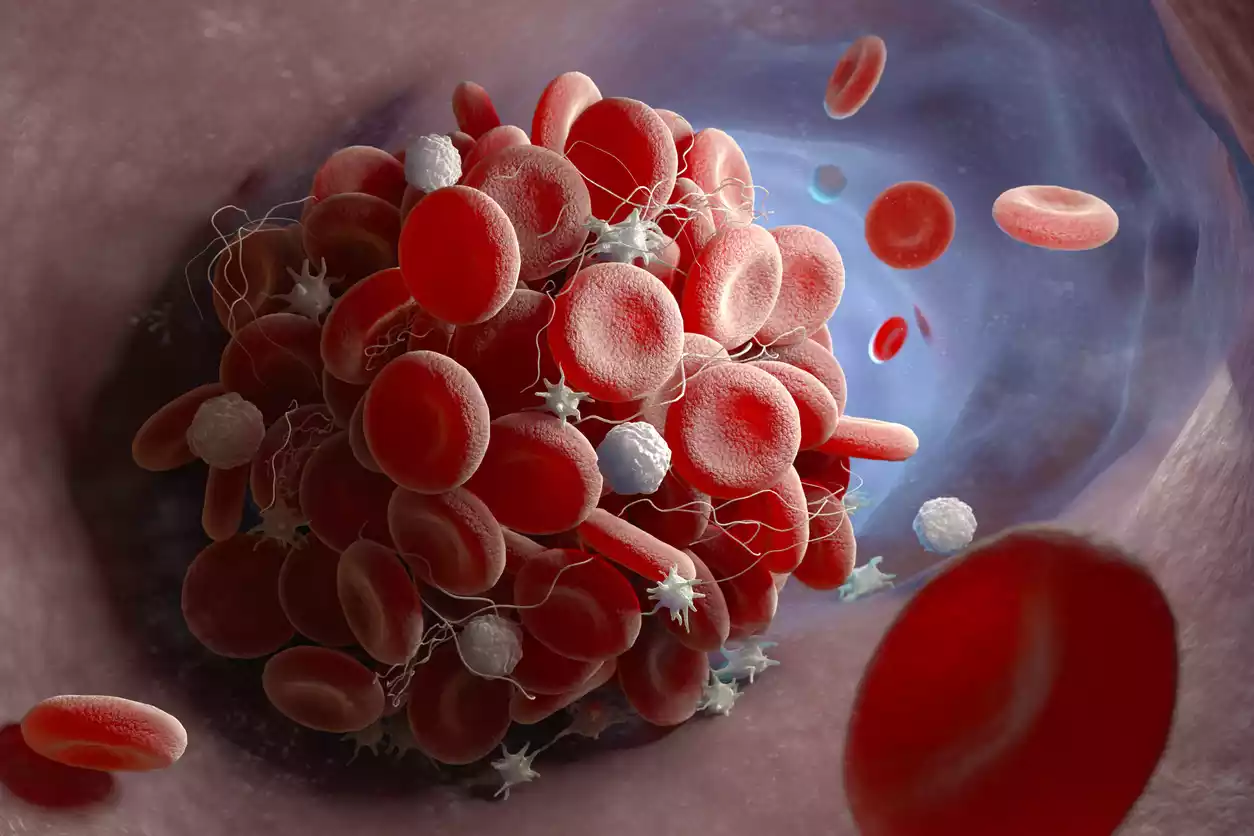
Types of Thrombus
Thrombus, or blood clot, can be classified into two primary types based on its location within the circulatory system:
- Arterial Thrombus: Arterial thrombosis occurs in the arteries, which carry oxygen-rich blood away from the heart. These clots can lead to conditions like heart attacks and strokes, causing damage to vital organs.
- Venous Thrombus: Venous thrombosis develops in the veins, responsible for returning oxygen-poor blood from various body tissues back to the heart. A common form of venous thrombosis is deep vein thrombosis (DVT), which can lead to pulmonary embolism if a piece of the clot dislodges and travels to the lungs.
Each type of thrombus has distinct causes, symptoms, and potential complications, requiring specific approaches to diagnosis and treatment.
Causes and Risk Factors
Understanding the causes and risk factors for thrombus formation is crucial for both prevention and management:
- Blood Stasis: Sluggish blood flow, often caused by immobility during long flights or bed rest, can increase the risk of thrombosis.
- Endothelial Injury: Damage to the inner lining of blood vessels can trigger clot formation. This damage can result from factors such as smoking, hypertension, or trauma.
- Hypercoagulability: Conditions that increase the tendency of blood to clot, such as genetic disorders or certain medications, can raise the risk of thrombosis.
- Age and Lifestyle: Advancing age and an unhealthy lifestyle, including a diet high in saturated fats, can contribute to a higher risk of thrombosis.
Symptoms of Thrombus
Signs of thrombosis vary depending on its extent and location, making its diagnosis all the more complex. Common symptoms include:
- Pain and Swelling: Pain and swelling, often localized to the affected area, are typical signs of thrombosis.
- Redness and Warmth: The skin over the clot may become red and warm to the touch.
- Shortness of Breath: In the case of pulmonary embolism, which can result from a venous thrombus, individuals may experience sudden shortness of breath, chest pain, and rapid heart rate.
- Neurological Symptoms: Arterial thrombosis can lead to symptoms such as weakness, numbness, and difficulty speaking if it causes a stroke.
Diagnosis and Treatment
Diagnosing and treating thrombosis is critical to prevent complications. Diagnostic procedures and treatment options include:
- Ultrasound: Doppler ultrasound is commonly used to diagnose venous thrombosis, providing real-time images of blood flow in the affected area.
- CT Scan: A computed tomography scan can help identify arterial thrombosis, including those in the brain or coronary arteries.
- Anticoagulation Therapy: Medications that thin the blood, such as heparin and warfarin, are used to prevent clot extension and reduce the risk of embolism.
- Thrombectomy: In severe cases, surgical removal of the thrombus may be necessary, particularly for arterial thrombosis.
- Compression Stockings: These can help prevent and manage venous thrombosis by improving blood flow in the legs.
Comparison table of Myxoma and Thrombus
Here’s a comparison table highlighting the key differences between Myxoma and Thrombus:
| Characteristic | Myxoma | Thrombus |
|---|---|---|
| Definition | Rare benign heart tumor | Blood clot in a blood vessel |
| Location | Primarily in the heart’s atria | Arteries or veins |
| Type | Tumor | Clot |
| Malignancy | Benign (non-cancerous) | Not applicable (non-cancerous) |
| Formation Mechanism | Abnormal cell growth | Blood coagulation process |
| Common Symptoms | Cardiovascular and systemic | Pain, swelling, redness, warmth, shortness of breath, neurological symptoms |
| Diagnostic Procedures | Echocardiography, cardiac MRI, CT scans, biopsy | Ultrasound, CT scan, blood tests |
| Treatment | Surgical removal | Anticoagulation therapy, thrombectomy, compression stockings |
| Preventive Measures | Regular cardiac check-ups, genetic counseling for those at risk | Physical activity, smoking cessation, healthy diet, hydration, compression stockings, medications |
| Potential Complications | Embolic events, heart valve dysfunction, recurrence | Pulmonary embolism, stroke, tissue damage, organ dysfunction |
| Prognosis | Positive following successful removal | Depends on location, size, and whether complications occur |
| Risk Factors | Familial predisposition, Carney Complex, age, and gender | Blood stasis, endothelial injury, hypercoagulability, age, and lifestyle |
This table provides a concise overview of the key differences between Myxoma and Thrombus, encompassing their nature, causes, symptoms, diagnosis, treatment, and preventive measures.
Similarities between Myxoma and Thrombus
While Myxoma and Thrombus are distinct cardiovascular conditions, they do share some similarities:
- Potential for Serious Complications: Both Myxoma and Thrombus can lead to severe health complications if not addressed promptly. Myxoma can result in cardiovascular issues and systemic symptoms, while Thrombus can lead to conditions such as heart attacks, strokes, or pulmonary embolism.
- Diagnostic Challenges: Diagnosing both conditions often requires a combination of clinical evaluation and medical imaging techniques. Echocardiography, CT scans, and other imaging modalities are commonly used for the diagnosis of both Myxoma and Thrombus.
- Need for Medical Intervention: Both conditions often require medical intervention for management. Myxoma usually necessitates surgical removal, while Thrombus may be treated with anticoagulant therapy, thrombectomy, or other medical interventions based on the specific case.
- Awareness and Early Detection: Early awareness of symptoms and timely medical attention are crucial for both Myxoma and Thrombus. Understanding the warning signs and seeking prompt medical care can significantly improve the prognosis for individuals affected by either condition.
Despite their differences, these shared aspects emphasize the importance of proactive healthcare and timely intervention in managing both Myxoma and Thrombus effectively.
Preventive Measures of Myxoma and Thrombus
Preventive measures for Myxoma and Thrombus differ due to the nature of these conditions:
Preventive Measures for Myxoma:
- Genetic Counseling: Individuals with a family history of Myxoma or a known genetic predisposition should consider genetic counseling to better understand their risk and potential preventive strategies.
- Regular Cardiac Check-Ups: Consult with a cardiologist for regular cardiac check-ups and screenings if you have a family history of Myxoma or are at risk.
- Healthy Lifestyle: While not a direct preventive measure, maintaining a healthy lifestyle can contribute to overall heart health. This includes regular exercise, a balanced diet, and avoiding smoking and excessive alcohol consumption.
- Awareness of Symptoms: Be aware of potential symptoms of Myxoma, such as cardiovascular issues, systemic symptoms, or neurological symptoms. Early recognition of symptoms can lead to earlier diagnosis and intervention.
Preventive Measures for Thrombus:
- Physical Activity: Engage in regular physical activity to promote healthy blood flow and reduce the risk of stasis, a common cause of Thrombosis. Move your legs during long flights or extended periods of immobility.
- Smoking Cessation: Do not smoke or expose yourself to second-hand smoke. Smoking can damage blood vessels and increase the risk of clot formation.
- Healthy Diet: Consume a diet low in saturated fats and high in fruits, vegetables, and whole grains to improve vascular health.
- Hydration: Stay well-hydrated to prevent blood from becoming too viscous.
- Compression Stockings: If at risk of Venous Thrombosis, consider the use of compression stockings to improve blood flow in the legs during prolonged periods of immobility.
- Medications: In some cases, doctors may prescribe anticoagulant medications to reduce the risk of clot formation, particularly for individuals with known risk factors.
It’s essential to consult with a healthcare provider to assess individual risk factors and determine the most suitable preventive strategies for both Myxoma and Thrombus.
Conclusion
Myxoma and Thrombus are distinct cardiovascular conditions with varying characteristics and implications. Myxoma is a rare benign heart tumor, often necessitating surgical removal, while Thrombus represents blood clots that can obstruct arteries or veins, leading to potentially life-threatening consequences. Early diagnosis and appropriate treatment are essential for both conditions.
Myxoma is challenging to prevent, but those at risk should consider regular cardiac check-ups. For Thrombus, preventive measures include lifestyle changes and, in some cases, anticoagulant therapy. Awareness and prompt medical attention are critical in managing these conditions effectively.