Anesthesia and Paresthesia are terms frequently used in the medical world but represent distinct concepts. Anesthesia refers to the deliberate induction of a loss or reduction of sensation, often to facilitate medical procedures without causing pain or discomfort. It can range from numbing a small area of the body to putting a patient into a state of unconsciousness. On the other hand, paresthesia is an abnormal sensation felt by an individual, often described as tingling, prickling, or a “pins and needles” feeling.
It is not intentionally induced but rather arises from various medical conditions or external factors affecting the nerves. While both relate to sensations in the body, they differ in their causes, mechanisms, and implications in healthcare.
What is Anesthesia?
Anesthesia is a medical procedure that uses drugs or agents to block or reduce sensations, allowing patients to undergo surgeries and other potentially painful procedures without experiencing pain or discomfort. The word “anesthesia” comes from the Greek words “an,” meaning “without,” and “aisthesis,” meaning “sensation.”
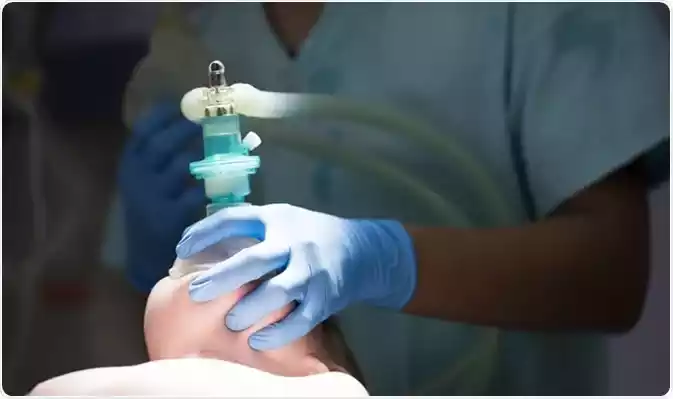
There are several types of anesthesia, each serving specific purposes:
- General Anesthesia: This type induces a complete loss of consciousness, ensuring that the patient doesn’t feel pain and doesn’t remember the surgical procedure. It affects the whole body, and the patient requires close monitoring of vital signs, as well as mechanical support for breathing.
- Regional Anesthesia: This type blocks sensation in a larger area of the body, such as an entire limb or the lower half of the body. Examples include epidural anesthesia (often used during childbirth) and spinal anesthesia.
- Local Anesthesia: Used to numb a small, specific area of the body. A patient remains conscious during the procedure. It’s often used for minor surgeries, dental work, or to insert a catheter or IV.
- Sedation: While not a type of anesthesia per se, sedation is used to relax a patient, reduce anxiety, or make them unaware of the procedure. It can range from minimal sedation, where a patient is relaxed but awake, to deep sedation, where a patient is on the edge of consciousness but can be awakened.
An anesthesiologist or nurse anesthetist typically administers anesthesia. These professionals monitor the patient’s vital signs, adjust the level of anesthesia as necessary, and ensure the patient’s safety and comfort throughout the procedure. After the procedure, patients might be observed in a recovery room, especially after general anesthesia, to ensure there are no adverse reactions as the anesthesia wears off.
What is Paresthesia?
Paresthesia refers to abnormal sensations in the skin, commonly described as tingling, prickling, “pins and needles”, or sometimes as burning or numbness. These sensations can occur without any apparent external stimulus and are typically felt in the extremities, such as the hands, feet, arms, or legs, but can occur elsewhere in the body.
There are various causes for paresthesia, including:
- Transient Paresthesia: This is temporary and can be due to a simple cause like sitting or lying in a position that compresses or puts pressure on a nerve, often referred to as the limb “falling asleep.”
- Chronic Paresthesia: This might indicate underlying neurological diseases or damage. Some common causes include:
- Nerve Entrapment Syndromes: Such as carpal tunnel syndrome.
- Neurological Diseases: Like multiple sclerosis or neuropathies.
- Stroke or Mini-stroke (Transient Ischemic Attack).
- Vitamin Deficiencies: Particularly B vitamins.
- Alcoholism: Due to its toxic effects on nerves.
- Diabetes: Resulting from diabetic neuropathy.
- Infections: Such as herpes zoster or Lyme disease.
- Certain Medications: That might have neuropathic side effects.
It’s important to distinguish between the sensation of paresthesia, which is often harmless and transient, and the symptom of an underlying condition. If someone experiences chronic or recurrent episodes of paresthesia, especially without a clear and harmless cause, it may warrant a medical evaluation to determine any potential underlying conditions or factors.
Comparison Table of Anesthesia and Paresthesia
Below the Comparison Table of Anesthesia and Paresthesia:
| Feature/Aspect | Anesthesia | Paresthesia |
|---|---|---|
| Definition | A medical procedure that uses drugs or agents to block or reduce sensations, allowing patients to undergo surgeries and other potentially painful procedures without pain. | Abnormal sensations in the skin, often described as tingling, prickling, or “pins and needles”. |
| Cause | Intentionally induced using drugs or agents. | Can be due to various causes, ranging from temporary nerve compression to underlying neurological diseases. |
| Duration | Typically temporary; lasts as long as the agent is active or until it wears off. | Can be transient (short-lived) or chronic (long-lasting). |
| Areas Affected | Can be localized, regional, or throughout the entire body, depending on the type. | Commonly felt in the extremities but can occur elsewhere. |
| Purpose | Used in medical settings to prevent pain or discomfort during procedures. | Typically an unintentional symptom indicating an underlying condition or temporary situation. |
| Management | Administered and monitored by healthcare professionals, such as anesthesiologists or nurse anesthetists. | Treatment or management is based on the underlying cause, which might require medical evaluation. |
| Examples | Local anesthesia (e.g., lidocaine injection), general anesthesia (e.g., inhalational agents like sevoflurane), regional anesthesia (e.g., epidural). | Transient paresthesia from “falling asleep” on an arm, chronic paresthesia from conditions like carpal tunnel syndrome or diabetic neuropathy. |
This table provides a concise comparison of anesthesia and paresthesia, highlighting their main distinctions and features.
The Link between Anesthesia and Paresthesia
The link between anesthesia and paresthesia primarily revolves around the potential complications or side effects that can arise from the administration of anesthetic agents or techniques. Here’s an exploration of the connection:
1. Direct Nerve Injury:
- When administering regional anesthesia, such as nerve blocks, there’s a risk of direct injury to the nerve with the needle. This injury can result in paresthesia.
2. Prolonged Pressure:
- During surgeries, especially lengthy ones, a patient’s position can compress a nerve for an extended period. This compression can lead to paresthesia postoperatively.
3. Tourniquet Paresthesia:
- During some surgeries, a tourniquet is applied to control bleeding. If it’s in place for an extended period, it can cause nerve ischemia and subsequent paresthesia.
4. Anesthetic Agents:
- Some anesthetic drugs, especially when given in large doses or when there’s prolonged exposure, can induce toxic reactions in peripheral nerves, leading to paresthesia.
5. Complications from Epidural or Spinal Anesthesia:
- Improper administration of epidural or spinal anesthesia can lead to nerve irritation or damage, resulting in paresthesia.
6. Previous Nerve Conditions:
- In patients with pre-existing nerve conditions or damage, anesthesia and the surgical procedure can exacerbate the condition, leading to postoperative paresthesia.
7. Intraneural Injection:
- Accidental injection of anesthetic agents directly into the nerve during regional blocks can result in paresthesia and nerve damage.
Prevention and Management:
- To reduce the risks associated with anesthesia-induced paresthesia, anesthesiologists use guidance techniques, like ultrasound or nerve stimulators, during nerve blocks. It ensures proper placement and minimizes nerve injury.
- Early detection and prompt management can prevent long-term complications. If a patient reports paresthesia postoperatively, it requires thorough evaluation to determine the cause and initiate appropriate management.
While anesthesia aims to prevent pain and discomfort during medical procedures, there is an inherent risk of complications, one of which is paresthesia. Proper technique, patient evaluation, and early intervention are crucial in mitigating these risks.
Dealing with Paresthesia Post-Anesthesia
Paresthesia post-anesthesia can be unsettling for patients, but understanding its potential causes and management strategies can be reassuring. Here are some considerations and approaches when dealing with post-anesthetic paresthesia:
1. Understand the Cause:
- Duration of Surgery: Prolonged surgeries, especially where the patient remains in one position for extended periods, can lead to nerve compression and subsequent paresthesia.
- Tourniquet Use: Extended application can cause nerve ischemia and subsequent paresthesia.
- Anesthetic Technique: Epidural, spinal, or regional anesthesia might cause temporary paresthesia, especially if there was any nerve irritation or direct injury during the procedure.
2. Immediate Interventions:
- Positional Changes: If paresthesia is due to the patient’s position during surgery, it will usually resolve upon changing the position postoperatively.
- Assess Circulation: Ensure there’s no circulatory compromise, especially if tourniquets were used.
- Monitor: Keep a close watch on the affected area, noting any changes in sensation, color, or temperature.
3. Pain Management:
- Analgesics: Over-the-counter pain relievers or prescribed medications can alleviate pain associated with paresthesia.
- Topical Treatments: Topical analgesics or patches may help in some cases.
4. Further Evaluation:
- If paresthesia persists or if there are other concerning symptoms, further evaluations like nerve conduction studies, MRI, or ultrasounds might be necessary to identify the exact cause and extent of the issue.
5. Long-term Management:
- Physical Therapy: Can be beneficial, especially if the paresthesia is due to nerve compression. Therapies can focus on exercises, stretches, and techniques to alleviate the compression or irritation.
- Medications: Certain medications, such as gabapentin or pregabalin, can be prescribed to manage neuropathic pain or symptoms associated with paresthesia.
6. Patient Reassurance:
- Communication: It’s crucial to communicate with the patient, explaining the potential causes and reassuring them that transient paresthesia post-anesthesia can be common and usually resolves on its own.
- Follow-up: Schedule regular follow-ups to monitor the condition and adjust treatment strategies as necessary.
7. Prevention in Future Procedures:
- If a patient experienced paresthesia after a procedure, special precautions should be taken in any subsequent surgeries or procedures. This might include using different anesthetic techniques, ensuring optimal positioning, or minimizing the duration of tourniquet application.
While paresthesia post-anesthesia can be concerning, understanding its potential causes, ensuring thorough evaluation, and implementing appropriate interventions can effectively manage and often resolve the issue. If you or someone you know experiences persistent paresthesia after a procedure, it’s essential to consult with a healthcare provider for a comprehensive assessment.
Conclusion
Anesthesia and Paresthesia, though distinct in their nature, can intersect in medical scenarios. Anesthesia is a deliberate medical intervention used to suppress sensations, allowing patients to undergo medical procedures without pain. On the other hand, paresthesia refers to the unexpected and often unsettling sensations of tingling or “pins and needles,” which can arise from various causes, including as a side effect or complication of anesthesia.
It’s crucial for medical professionals to understand this relationship, employ preventive measures, and manage potential complications to ensure patient safety and comfort. Through careful administration, patient education, and continuous monitoring, the risks associated with post-anesthetic paresthesia can be significantly reduced.