Coinfection and Superinfection refer to the presence of multiple pathogens within a host organism. Coinfection occurs when a host is simultaneously infected by two or more pathogens, either at the same time or in close succession. This simultaneous presence can influence the progression of diseases, their severity, and treatment responses.
Superinfection, on the other hand, describes a scenario where a host that is already infected by a primary pathogen subsequently becomes infected by a different strain or species of pathogen, often with implications on treatment strategies or disease prognosis. Both phenomena highlight the complex interactions that can occur between different pathogens within a single host and the importance of understanding these interactions in clinical settings.
What is Coinfection?
Coinfection refers to the simultaneous infection of a host by two or more pathogens. These pathogens can be of the same species or different species. Coinfection can occur when a host is exposed to multiple pathogens nearly simultaneously, or when a secondary pathogen infects an already infected host before the first infection has resolved.
Understanding coinfection is crucial in epidemiology and clinical medicine, as the presence of multiple pathogens can influence disease progression, severity, immune response, and treatment outcomes.
Characteristics of Coinfection
Coinfection involves the simultaneous infection of a host by two or more pathogens. Here are its main characteristics:
- Multiple Pathogens: By definition, coinfection means the presence of two or more pathogens infecting a host either at the same time or in close succession.
- Variability in Pathogens: The pathogens in a coinfection can be of the same species (homologous coinfection) or different species (heterologous coinfection).
- Disease Interactions: Coinfections can lead to various interactions in terms of disease manifestation:
- Synergistic: One infection exacerbates the symptoms or progression of another.
- Antagonistic: One infection hinders or reduces the effects of another.
- Neutral: The infections don’t significantly influence each other.
- Immune Response Modulation: Coinfections can alter the host’s immune response. For instance, one pathogen might suppress specific immune functions that could either aid or hinder the proliferation of the second pathogen.
- Treatment Complications: Coinfected patients may require multifaceted treatment approaches to address each pathogen, leading to potential drug interactions or challenges in managing treatment side effects.
- Diagnostic Challenges: Coinfections can make diagnosis more complex, especially if the symptoms of one infection overlap or mask those of another.
- Transmission Dynamics: Coinfections might influence transmission dynamics, especially if one pathogen alters the host’s behavior or susceptibility to another.
- Evolutionary Implications: Coinfections can drive the evolution of pathogens, particularly if there’s competition or cooperation between them. This can influence virulence, resistance, and other pathogen traits.
- Clinical Prognosis: The presence of multiple pathogens can alter the prognosis of diseases. For instance, certain coinfections can either exacerbate or mitigate the severity of one or both diseases.
Understanding these characteristics of coinfection is crucial for effective clinical management, disease control, and epidemiological studies.
Real-world examples of Coinfection
Coinfections are relatively common in various parts of the world and can result from simultaneous infections by viruses, bacteria, parasites, or a combination of these agents. Here are some real-world examples of coinfections:
- HIV and Tuberculosis (TB): One of the most significant global health challenges is the coinfection of HIV and TB. HIV suppresses the immune system, making individuals more susceptible to TB infections. Conversely, TB can accelerate the progression of HIV.
- Malaria and Dengue: Both are mosquito-borne diseases that can coexist in many tropical regions. It’s possible for individuals to be coinfected with both malaria (caused by Plasmodium parasites) and dengue (caused by the dengue virus).
- COVID-19 and Influenza: Especially during flu seasons, individuals can be infected with both the SARS-CoV-2 virus (causing COVID-19) and influenza viruses. This coinfection can pose significant challenges in diagnosis and treatment.
- Hepatitis B and Hepatitis C: Both are viral infections affecting the liver. It’s possible for individuals, especially those with certain risk factors like intravenous drug use, to be coinfected with both hepatitis B virus (HBV) and hepatitis C virus (HCV).
- Lyme Disease and Babesiosis: In areas endemic for ticks, individuals can get bitten by ticks carrying both the bacteria responsible for Lyme disease (Borrelia burgdorferi) and the parasites causing babesiosis (Babesia spp.).
- HIV and Hepatitis C: Among certain populations, especially intravenous drug users, coinfection with HIV and HCV is common. Both viruses can be transmitted through shared needles.
- Tuberculosis and Influenza: It’s possible for individuals with active TB to contract influenza. This coinfection can exacerbate respiratory symptoms and complicate treatment.
- HIV and Malaria: In regions where both HIV and malaria are endemic, coinfections can occur. HIV can make an individual more susceptible to severe malarial symptoms, and malaria can increase the viral load of HIV.
These examples highlight the complexities and challenges posed by coinfections. Effective public health strategies need to consider the potential overlap of various pathogens in specific regions or populations.
What is Superinfection?
Superinfection refers to the infection of a host by a secondary pathogenic agent while the host is already infected by a primary pathogen. This secondary infection is distinct from and typically follows the primary infection, often after the primary pathogen has weakened the host’s defenses. The secondary pathogen can be a different strain or species from the primary pathogen.
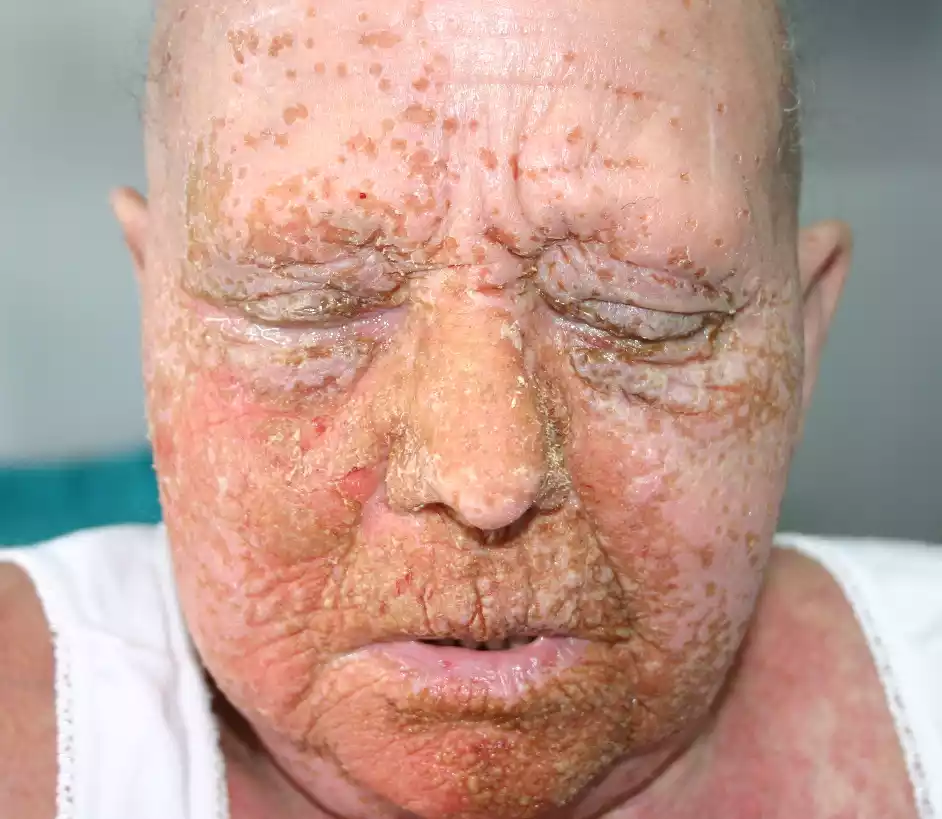
Superinfections are particularly noteworthy because they can be more severe or harder to treat, especially if the host’s immune system is already compromised by the initial infection or if treatment for the primary infection inadvertently promotes the secondary infection.
Characteristics of Superinfection
Superinfection refers to a scenario where an individual who is already infected with a primary pathogen becomes subsequently infected by a different pathogen. Here are its main characteristics:
- Sequential Infections: In superinfection, the secondary infection follows an initial or primary infection. The timing might vary, but there is a clear sequence.
- Different Pathogens: The secondary pathogen in a superinfection is typically distinct from the primary pathogen. It can be a different strain or an entirely different species.
- Compromised Host Defense: Often, the primary infection weakens the host’s immune defenses in some manner, making the host more susceptible to a secondary infection.
- Enhanced Severity: Superinfections can be more severe or challenging to treat, especially if the host’s immune response is already compromised by the initial infection.
- Treatment Implications: Treatment for the primary infection might inadvertently promote the secondary infection. For instance, the use of antibiotics might lead to a fungal superinfection due to the disruption of normal microbial flora.
- Diagnostic Challenges: Superinfections can complicate diagnosis. The secondary infection might be mistaken as a complication or exacerbation of the primary infection.
- Variability in Manifestations: The clinical manifestations of superinfections can vary widely. They can present with entirely new symptoms, or they might exacerbate the symptoms of the primary infection.
- Resistance Issues: Especially in bacterial superinfections, the secondary bacteria might be resistant to the antibiotics being used to treat the primary bacterial infection.
- Epidemiological Significance: Superinfections can have significant epidemiological implications, especially in settings where primary pathogens are widespread, and individuals are at risk of exposure to multiple pathogens.
Understanding superinfection is crucial in clinical settings to anticipate potential complications or challenges in disease management and treatment. Recognizing superinfections early can make a significant difference in patient outcomes.
Real-world examples of Superinfection
Superinfection refers to the occurrence of a secondary infection in a person who is already infected with a different pathogen. Here are some real-world examples of superinfections:
- Bacterial Superinfection following Viral Infections: A classic example is a person who, after contracting a viral infection like the flu (influenza), subsequently develops a bacterial pneumonia caused by bacteria like Streptococcus pneumoniae or Staphylococcus aureus. The primary viral infection can damage the respiratory tract lining and compromise defenses, allowing bacteria to invade and establish an infection.
- Fungal Infections after Antibiotic Treatment: Broad-spectrum antibiotics can kill off the normal flora of the gut, allowing opportunistic fungi, like Candida, to overgrow. This can lead to oral thrush or vaginal yeast infections as a superinfection following antibiotic treatment.
- Drug-resistant Bacterial Superinfections: In hospital settings, prolonged treatment with certain antibiotics can lead to superinfections with drug-resistant bacteria like methicillin-resistant Staphylococcus aureus (MRSA) or vancomycin-resistant enterococci (VRE).
- HIV Superinfection: This refers to an individual with HIV getting infected with a second strain of the virus. The two strains can recombine, potentially leading to a more aggressive or drug-resistant form of the virus.
- Herpes Superinfection: An individual with atopic dermatitis (eczema) can develop a widespread herpes infection known as eczema herpeticum if they get infected with the herpes simplex virus.
- Secondary Bacterial Infections after Viral Conjunctivitis: A person with viral conjunctivitis (pink eye) can develop a secondary bacterial infection if bacteria invade the already inflamed and compromised eye.
These real-world examples highlight the importance of early diagnosis and intervention, as superinfections can often be more severe than the primary infection and may require different therapeutic strategies.
Comparison table of Coinfection and Superinfection
Here’s a comparison table of Coinfection and Superinfection:
| Aspect | Coinfection | Superinfection |
|---|---|---|
| Definition | Simultaneous infection of a host by two or more pathogens, either of the same species or different species. | Infection of a host by a secondary pathogenic agent after or during an ongoing infection by a primary pathogen. |
| Timing | Multiple pathogens infect the host around the same time or in close succession. | A secondary infection follows or occurs during a primary infection. |
| Pathogen Species | Can be the same species (homologous) or different species (heterologous). | Typically a different strain or species from the primary pathogen. |
| Impact on Disease | Interactions between pathogens can be synergistic, antagonistic, or neutral, affecting disease severity and progression. | The secondary infection can be more severe, especially if the host’s defenses are compromised by the primary infection. |
| Treatment Concerns | Treatment may need to address multiple pathogens, considering drug interactions or competing pathogenic strategies. | Treatment of the primary infection might inadvertently promote the secondary one, especially if the secondary agent is resistant. |
This table provides a concise overview of the distinctions between coinfection and superinfection. In practice, understanding these differences is crucial for correct diagnosis, treatment, and prognosis.
What are the similarities between Coinfection and Superinfection?
Both coinfection and superinfection involve the presence of multiple pathogens within a single host, leading to complexities in disease progression, diagnosis, and treatment. Here are the similarities between the two:
- Multiple Pathogens: Both coinfection and superinfection involve the host being infected by more than one pathogenic agent.
- Disease Progression: The presence of multiple pathogens can influence the progression and severity of the disease. In both scenarios, interactions between pathogens can lead to heightened disease severity or modified symptoms.
- Treatment Challenges: Both conditions can complicate the treatment process. With multiple pathogens present, treatment may need to account for each pathogen separately, and there’s a potential for drug interactions or conflicting treatment strategies.
- Diagnostic Complexity: Identifying and differentiating between multiple pathogens can be challenging, especially when symptoms overlap or when one infection masks the symptoms of another.
- Immune Response: The host’s immune system may respond differently or be overwhelmed when faced with multiple pathogens, leading to potential complications in the host’s ability to fight off the infections.
- Epidemiological Concerns: Both coinfections and superinfections are of epidemiological significance. Understanding the dynamics of how pathogens spread and interact within hosts is crucial for disease control and prevention strategies.
While coinfection and superinfection have these similarities, it’s also essential to remember their differences, particularly regarding the timing and sequence of infections.
Medical Implications of Coinfection and Superinfection
Coinfections and superinfections present unique challenges in the medical field, spanning from diagnosis to treatment. Here are the medical implications of both:
Coinfection:
- Diagnostic Complexity: Coinfections can make diagnosis more intricate since symptoms may overlap, or one infection may mask the symptoms of another. Identifying multiple pathogens requires a broader array of diagnostic tests.
- Treatment Challenges: Treating multiple pathogens may necessitate a combination of drugs, leading to potential drug interactions or heightened side effects. Additionally, treatment for one pathogen might not be effective, or could even be detrimental, for the other.
- Altered Disease Progression: The presence of multiple pathogens can influence disease severity. Interactions between pathogens can be synergistic, leading to a more severe disease course, or antagonistic, potentially mitigating symptoms.
- Immune System Overload: The body’s immune response may become overwhelmed or misdirected, which can lead to a more severe disease or longer recovery time.
- Epidemiological Impact: Coinfections can influence transmission rates, especially if one pathogen affects the host’s susceptibility or exposure to another.
Superinfection:
- Increased Disease Severity: Superinfections often occur because the primary infection has weakened the body’s defenses, making the secondary infection potentially more severe.
- Treatment Complications: The treatment for the primary infection might reduce the body’s ability to fend off a secondary pathogen. For instance, antibiotics can disrupt the body’s normal flora, paving the way for fungal superinfections.
- Resistance Concerns: Especially in hospital settings, superinfections can be caused by drug-resistant strains that are harder to treat, such as MRSA following antibiotic treatments.
- Diagnostic Challenges: As with coinfections, the symptoms of the primary infection might overshadow or be confused with those of the superinfection, complicating diagnosis.
- Extended Hospital Stay: Superinfections, particularly those acquired in hospitals, can lead to extended hospital stays, increasing healthcare costs and the risk of additional complications.
- Immune Response Complexity: A superinfection can complicate the body’s immune response, as the immune system has to combat multiple pathogens sequentially, which might hinder effective response to the secondary pathogen.
For clinicians, understanding the potential for coinfections and superinfections is crucial. They must consider broader diagnostic approaches, be cautious with treatments that might predispose patients to secondary infections, and stay updated with current knowledge on potential pathogen interactions.
Prevention and Control
Preventing and controlling coinfections and superinfections are paramount in healthcare to reduce morbidity and mortality, as well as to curb the spread of infectious diseases. The strategies often overlap but are tailored based on the specific pathogens involved and the populations at risk.
Prevention:
- Vaccination: If vaccines are available for the infectious agents in question, ensuring high coverage can significantly reduce the risk of infections. Examples include vaccines for influenza, hepatitis B, and pneumonia.
- Antimicrobial Stewardship: This refers to coordinated interventions designed to improve and measure the appropriate use of antimicrobial agents. It aims to ensure effective treatment of infections, reduce overuse of antibiotics, and combat antibiotic resistance, which is a significant factor in superinfections.
- Hand Hygiene: Regular handwashing with soap and water or using an alcohol-based hand sanitizer can significantly reduce the transmission of many pathogens.
- Use of Barrier Methods: For sexually transmitted infections, the use of condoms can reduce the risk of coinfections (like HIV and herpes or HPV).
- Safe Practices: Ensuring safe practices, such as safe injection practices among healthcare workers and drug users, can prevent multiple infections.
- Environmental Control: This includes measures like vector control for mosquito-borne diseases (e.g., bed nets for malaria prevention and eliminating stagnant water for dengue prevention).
Control:
- Isolation and Quarantine: Isolating infected individuals can prevent the spread of infections to others. Quarantine refers to separating and restricting the movement of individuals exposed to an infectious disease.
- Surveillance: Active surveillance of infectious diseases can help in early detection, allowing for timely interventions to prevent wider outbreaks.
- Education: Informing the public about the risks and prevention methods of specific infections can lead to safer individual behaviors.
- Access to Healthcare: Ensuring prompt access to medical care allows for early diagnosis and treatment, reducing the spread of infections and the risk of complications.
- Treatment: Effective and timely treatment, especially for primary infections, can reduce the risk of superinfections. For HIV patients, antiretroviral therapy (ART) reduces viral load, thus decreasing the risk of opportunistic infections.
- Infection Control in Healthcare Settings: This includes measures like sterilization of medical equipment, proper hand hygiene protocols, and use of personal protective equipment (PPE) to prevent hospital-acquired infections and superinfections.
- Contact Tracing: Identifying and managing individuals who have come into contact with an infected person can control the spread of infections.
- Reporting: Healthcare providers and laboratories should report certain infections to health departments, facilitating more extensive control measures.
The strategies for prevention and control of coinfections and superinfections necessitate a multi-pronged approach involving individuals, communities, healthcare providers, and policymakers. Effective measures can lead to significant reductions in disease burden and associated complications.
Impacts on Public Health
Coinfections and superinfections can have profound implications on public health. The intersection of multiple pathogens in a host, whether simultaneously or sequentially, can compound disease burden, complicate medical interventions, and strain healthcare systems. Here are some of the impacts of coinfections and superinfections on public health:
- Increased Morbidity and Mortality: Coinfections can lead to more severe clinical outcomes, as the presence of multiple pathogens might amplify disease symptoms or accelerate disease progression. Superinfections often arise in a context where the primary infection has already compromised the host, leading to heightened susceptibility and potentially worse outcomes.
- Complex Disease Management: Coinfections can complicate treatment regimens. In some cases, treatments for one infection might interfere with treatments for another, or worsen the clinical course of the second disease. This complexity requires more advanced medical expertise and careful monitoring.
- Economic Impact: Increased hospital stays, more complex treatments, and the heightened need for diagnostic tests can escalate healthcare costs. On a broader scale, coinfections and superinfections can impact workforce productivity and economic growth, particularly if they affect a significant portion of the population.
- Strain on Healthcare Systems: Healthcare facilities may face an influx of patients with more severe symptoms, requiring more intensive care or longer hospitalization. This can strain resources, especially in regions with limited healthcare infrastructure.
- Challenges in Surveillance and Reporting: Distinguishing coinfections from single infections, especially when symptoms overlap, can present challenges in disease surveillance. This can lead to underreporting or misclassification, affecting the accuracy of public health data.
- Impediments to Eradication Efforts: Coinfections can hinder efforts to control or eradicate specific diseases. For instance, in areas where both malaria and HIV are prevalent, HIV-related immunosuppression can increase the risk of severe malaria.
- Increased Antibiotic Resistance: Superinfections often involve drug-resistant strains, particularly in hospital settings. This can result from the overuse or misuse of antibiotics during the treatment of the primary infection.
- Health Inequities: Vulnerable populations, such as those with limited access to healthcare, the economically disadvantaged, or those living in regions with high disease prevalence, may be disproportionately affected by coinfections and superinfections. This can exacerbate existing health inequities.
- Complicated Vaccine Strategies: In regions with prevalent coinfections, vaccine strategies might need to account for potential interactions between pathogens or their respective vaccines.
- Public Awareness and Behavior: Coinfections can influence public perceptions about diseases and their risks. This can affect behaviors, compliance with treatment, and participation in prevention efforts.
Given these substantial public health impacts, it’s crucial for health systems, policymakers, researchers, and communities to be aware of the risks of coinfections and superinfections and to develop strategies to prevent, detect, and manage them effectively.
Conclusion
Coinfections and superinfections represent complex interactions of multiple pathogens within a host. While coinfections involve simultaneous infections by different pathogens, superinfections occur sequentially, often exploiting the vulnerabilities introduced by the primary infection. Both conditions can amplify disease severity, complicate clinical management, and pose significant challenges to public health. Understanding the dynamics and implications of these multi-pathogen infections is crucial for effective diagnosis, treatment, and prevention strategies.