Kussmaul and Cheyne Stokes are two distinct abnormal breathing patterns that provide crucial insights into a person’s health. Kussmaul respiration is characterized by deep, rapid, and labored breathing, often associated with metabolic acidosis. Cheyne-Stokes respiration exhibits an alternating pattern of deep, quick breaths and periods of apnea, typically linked to neurological and cardiac conditions. Understanding these respiratory patterns is essential for healthcare professionals as they can serve as valuable diagnostic clues and guide appropriate treatment strategies.
What is Kussmaul?
Kussmaul respiration is a type of abnormal breathing pattern characterized by deep, rapid, and labored breaths. It typically occurs as a compensatory response to metabolic acidosis, a condition characterized by an excess of acid in the body’s fluids.
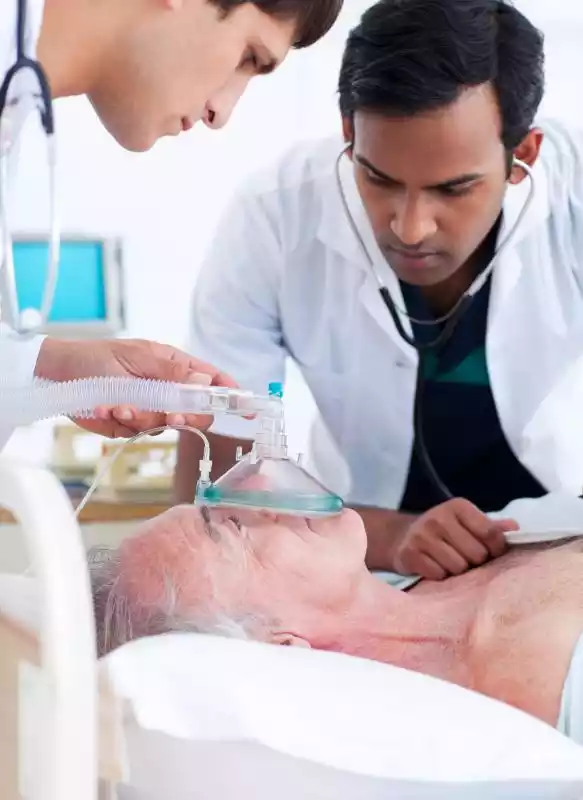
Kussmaul respiration helps the body attempt to eliminate excess acid by increasing the rate and depth of breathing, thereby expelling more carbon dioxide and potentially restoring the body’s acid-base balance. This respiratory pattern is often associated with medical conditions such as diabetic ketoacidosis, renal failure, and various metabolic disorders.
Causes of Kussmaul
Kussmaul respiration is a specific abnormal breathing pattern characterized by deep, rapid, and labored breaths. It is typically associated with metabolic acidosis, which is a condition characterized by an excess of acid in the body’s fluids.
The primary causes of Kussmaul respiration include:
- Diabetic Ketoacidosis (DKA): This is one of the most common causes of Kussmaul respiration. DKA occurs in individuals with uncontrolled diabetes when there is a shortage of insulin, leading to the breakdown of fatty acids and the production of acidic ketones.
- Renal Failure: Kidney dysfunction can lead to the accumulation of acids in the body, resulting in metabolic acidosis and Kussmaul respiration.
- Metabolic Disorders: Various metabolic disorders, such as lactic acidosis or severe dehydration, can disrupt the body’s acid-base balance, leading to Kussmaul respiration.
- Toxic Ingestions: Ingesting certain toxic substances or overdosing on medications can cause metabolic disturbances that result in Kussmaul respiration.
- Sepsis: Severe infections, especially those progressing to septic shock, can disrupt metabolic processes and lead to metabolic acidosis and Kussmaul breathing.
- Hyperventilation: Sometimes, individuals may hyperventilate voluntarily or involuntarily in response to anxiety, panic attacks, or other psychological stressors. This can mimic Kussmaul respiration but is not associated with metabolic acidosis.
It’s crucial to identify and address the underlying cause of Kussmaul respiration because it often indicates a severe medical condition. Prompt diagnosis and treatment are essential to address the root cause and restore normal breathing patterns.
Symptoms of Kussmaul
Kussmaul respiration is primarily a distinctive abnormal breathing pattern characterized by deep, rapid, and labored breaths. While it is primarily a respiratory pattern, Kussmaul respiration is typically observed in the context of an underlying medical condition, and its symptoms may vary depending on the cause.
Some common symptoms and signs associated with Kussmaul respiration and its underlying causes include:
- Deep, Rapid, and Labored Breathing: The hallmark symptom of Kussmaul respiration is the patient’s breathing pattern, which is deep (hyperpnea), rapid (tachypnea), and often associated with audible sighing or gasping.
- Increased Respiratory Rate: Patients with Kussmaul respiration will have an elevated respiratory rate as they try to compensate for metabolic acidosis.
- Fatigue: Individuals may experience fatigue and exhaustion due to the increased effort required for breathing.
- Confusion: In cases of severe metabolic acidosis, patients may exhibit confusion, altered mental status, or even loss of consciousness.
- Thirst: Dehydration is often associated with metabolic acidosis, leading to increased thirst.
- Nausea and Vomiting: Patients may experience gastrointestinal symptoms like nausea and vomiting.
- Abdominal Pain: In cases of diabetic ketoacidosis (a common cause of Kussmaul respiration), abdominal pain may be present.
- Fruity Breath Odor: In diabetic ketoacidosis, the breath may have a fruity or acetone-like odor due to the presence of ketones.
- Electrolyte Imbalances: Kussmaul respiration is often accompanied by disturbances in electrolyte levels, such as high blood sugar levels (hyperglycemia) in diabetic ketoacidosis.
Kussmaul respiration itself is a compensatory mechanism in response to metabolic acidosis, so it is a symptom rather than a condition in itself. The focus of treatment should be on identifying and addressing the underlying cause of metabolic acidosis, which, in turn, will help alleviate the symptoms associated with Kussmaul respiration. If you or someone you know is experiencing these symptoms, seek immediate medical attention, as Kussmaul respiration can be a sign of a serious medical condition.
What is Cheyne Stokes?
Cheyne-Stokes respiration is an abnormal breathing pattern characterized by a cyclical and gradual waxing and waning of both the depth and rate of breathing. It involves a sequence of progressively deeper and faster breaths followed by a period of apnea, during which the person temporarily stops breathing. This pattern repeats in a rhythmic cycle.
Cheyne-Stokes respiration is typically associated with certain medical conditions, especially those affecting the central nervous system or the cardiovascular system, such as heart failure, stroke, and traumatic brain injury. It is important for healthcare professionals to recognize Cheyne-Stokes respiration as it can be indicative of underlying health issues and may require specific medical management.
Causes of Cheyne Stokes
Cheyne-Stokes respiration is an abnormal breathing pattern characterized by a cyclical and gradual waxing and waning of both the depth and rate of breathing, with periods of apnea (temporary cessation of breathing). It is typically associated with underlying medical conditions, particularly those affecting the central nervous system or the cardiovascular system.
Common causes of Cheyne-Stokes respiration include:
- Heart Failure: Cheyne-Stokes respiration is often observed in individuals with congestive heart failure. The compromised heart function can lead to fluctuations in blood oxygen levels and trigger this breathing pattern.
- Stroke: Brain injuries, including strokes, can disrupt the normal control of breathing, leading to Cheyne-Stokes respiration. This is particularly common in cases where the stroke affects the brainstem or areas responsible for respiratory control.
- Traumatic Brain Injury: Severe head injuries that damage the brain’s respiratory control centers can result in Cheyne-Stokes respiration.
- Brain Tumors: Tumors in the brain, especially those that impinge on areas involved in breathing regulation, can lead to this abnormal respiratory pattern.
- High-Altitude Hypoxia: At high altitudes, individuals may develop Cheyne-Stokes respiration as a response to reduced oxygen availability in the air, although this is not typically associated with underlying medical conditions.
- Opioid Medications: Some opioid medications, such as morphine, can depress the respiratory centers in the brain, leading to Cheyne-Stokes respiration.
- Congenital Central Hypoventilation Syndrome (CCHS): This rare genetic disorder affects the autonomic nervous system’s control over breathing, leading to abnormal respiratory patterns, including Cheyne-Stokes respiration.
- Aging: In some elderly individuals, Cheyne-Stokes respiration can occur as a result of age-related changes in respiratory control.
- Sleep-Related Disorders: Conditions like sleep apnea or central sleep apnea can result in Cheyne-Stokes respiration during sleep.
It’s essential to recognize Cheyne-Stokes respiration as it can indicate an underlying medical problem, often a serious one. Identifying and addressing the cause of Cheyne-Stokes respiration is crucial for proper management and treatment of the underlying condition. Individuals experiencing this breathing pattern should seek medical evaluation and care.
Symptoms of Cheyne Stokes
Cheyne-Stokes respiration is primarily characterized by a distinctive abnormal breathing pattern, which includes a cyclical and gradual waxing and waning of both the depth and rate of breathing, alternating with periods of apnea (temporary cessation of breathing). While Cheyne-Stokes respiration itself is a respiratory pattern, it typically occurs in the context of an underlying medical condition.
Some common symptoms and signs associated with Cheyne-Stokes respiration and its underlying causes include:
- Abnormal Breathing Pattern: The hallmark symptom is the rhythmic and cyclical breathing pattern, where breathing gradually increases in depth and rate before decreasing and eventually pausing during apnea episodes.
- Snoring: Individuals with Cheyne-Stokes respiration, especially during sleep, may produce loud snoring or irregular noises as they breathe.
- Daytime Sleepiness: The interrupted sleep caused by Cheyne-Stokes respiration can lead to daytime fatigue and excessive sleepiness.
- Insomnia: Sleep disturbances, including difficulty falling asleep or staying asleep, are common in individuals with this condition.
- Cognitive Impairment: Some individuals may experience cognitive symptoms such as memory problems, difficulty concentrating, or confusion due to the disrupted sleep patterns.
- Increased Heart Rate: Cheyne-Stokes respiration can be associated with an increased heart rate (tachycardia) during the periods of increased breathing.
- Swelling in the Legs and Ankles: In cases where heart failure is the underlying cause, individuals may experience fluid retention, leading to swelling in the legs and ankles.
- Shortness of Breath: Patients may report episodes of shortness of breath, especially during the periods of increased breathing.
- Fatigue: The disrupted sleep and oxygen fluctuations can result in persistent fatigue and reduced physical endurance.
Cheyne-Stokes respiration itself is a manifestation of an underlying medical condition, often related to heart or brain function. Therefore, addressing the cause of Cheyne-Stokes respiration is crucial for proper management and treatment of the associated symptoms. If you or someone you know is experiencing these symptoms, particularly the abnormal breathing pattern, seek immediate medical evaluation and care to determine and address the underlying cause.
Comparison Table of Kussmaul and Cheyne Stokes
Here’s a comparison table highlighting the key differences between Kussmaul respiration and Cheyne-Stokes respiration:
| Aspect | Kussmaul Respiration | Cheyne-Stokes Respiration |
|---|---|---|
| Definition | Deep, rapid, and labored breathing | Cyclical, gradual changes in breath rate and depth with periods of apnea |
| Breathing Pattern | Deep, rapid, and continuous breaths | Cyclical, alternating between deep, rapid breaths and apnea |
| Associated Conditions | Metabolic acidosis (e.g., diabetic ketoacidosis, renal failure, metabolic disorders) | Underlying medical conditions affecting the central nervous system or cardiovascular system (e.g., heart failure, stroke, brain injury) |
| Clinical Significance | Compensatory response to metabolic acidosis; can be life-threatening if untreated | Indicator of severe underlying medical issues; may precede death in some cases |
| Primary Causes | Metabolic acidosis, kidney dysfunction, metabolic disorders, toxic ingestions, sepsis | Heart failure, stroke, traumatic brain injury, brain tumors, high-altitude hypoxia, opioid medications, congenital central hypoventilation syndrome (CCHS), aging |
| Symptoms | – Deep, rapid breaths
– Increased respiratory rate – Fatigue – Confusion (in severe cases) – Thirst (associated with some causes) – Nausea and vomiting (associated with some causes) |
– Cyclical breathing pattern
– Snoring or irregular noises – Daytime sleepiness – Insomnia – Cognitive impairment (memory problems, difficulty concentrating) – Increased heart rate (during periods of increased breathing) – Swelling in the legs and ankles (associated with heart failure) – Shortness of breath (during periods of increased breathing) – Fatigue |
| Treatment Approach | Identify and treat the underlying cause; correct acid-base imbalance | Identify and manage the primary medical condition; may involve supplemental oxygen in some cases |
Understanding these differences is crucial for healthcare professionals as they help in the recognition and appropriate management of patients exhibiting these abnormal respiratory patterns.
What is the similarities between Kussmaul and Cheyne Stokes?
While Kussmaul respiration and Cheyne-Stokes respiration are distinct abnormal breathing patterns associated with different underlying conditions, they do share some similarities:
- Abnormal Breathing Patterns: Both Kussmaul and Cheyne-Stokes respiration are characterized by abnormal breathing patterns that deviate from normal, steady, and rhythmic breathing.
- Cyclical Nature: Both patterns involve a cyclical rhythm in breathing. In Kussmaul respiration, this cycle consists of rapid, deep breaths without apnea. In Cheyne-Stokes respiration, the cycle includes alternating phases of increasing and decreasing breath depth and rate with periods of apnea.
- Clinical Significance: Both patterns can serve as important clinical signs. They indicate underlying medical issues and often prompt healthcare professionals to investigate and identify the root cause.
- Potential Seriousness: Both patterns, when observed, can be indicative of serious medical conditions. Kussmaul respiration may signal severe metabolic disturbances, while Cheyne-Stokes respiration may be associated with neurological or cardiac disorders, some of which can be life-threatening if not properly managed.
- Importance of Prompt Evaluation: In both cases, it is crucial for healthcare providers to promptly evaluate and assess the patient, identify the underlying cause, and initiate appropriate treatment. Early intervention can significantly impact patient outcomes.
Despite these similarities, it is essential to recognize that the underlying causes, characteristics, and management of Kussmaul and Cheyne-Stokes respiration are distinct, requiring specific approaches tailored to each condition. Therefore, while the breathing patterns share some commonalities, they remain separate clinical entities with unique clinical implications.
Diagnosing Kussmaul and Cheyne-Stokes Breathing
Diagnosing Kussmaul and Cheyne-Stokes breathing patterns involves a combination of clinical assessment, medical history, physical examination, and diagnostic tests to identify the underlying causes.
Here are the steps and considerations for diagnosing each:
Diagnosing Kussmaul Breathing:
- Clinical Assessment: The healthcare provider will first conduct a thorough clinical assessment, including taking a detailed medical history and performing a physical examination. They will inquire about symptoms like rapid, deep, and labored breathing.
- Measurement of Vital Signs: Vital signs, including respiratory rate, heart rate, blood pressure, and temperature, will be measured and monitored to assess the patient’s overall condition.
- Arterial Blood Gas (ABG) Analysis: An ABG test is crucial for diagnosing Kussmaul breathing. It measures the levels of oxygen and carbon dioxide in the blood, as well as the pH balance. Kussmaul respiration is often associated with metabolic acidosis, which will be reflected in the ABG results.
- Blood Glucose Measurement: If there is a suspicion of diabetic ketoacidosis as the cause of Kussmaul respiration, blood glucose levels will be checked to confirm hyperglycemia.
- Electrolyte Panel: An electrolyte panel may be performed to assess for imbalances associated with metabolic acidosis.
- Urinalysis: In cases of suspected diabetes or renal dysfunction, a urinalysis may be conducted to check for ketones and other abnormalities.
- Imaging and Additional Tests: Depending on the suspected cause and the patient’s overall condition, imaging studies (e.g., chest X-ray, CT scan) and additional tests may be ordered to identify underlying conditions.
Diagnosing Cheyne-Stokes Respiration:
- Clinical Assessment: As with Kussmaul breathing, a clinical assessment is the initial step. A detailed medical history and physical examination are performed to identify the presence of Cheyne-Stokes respiration and any associated symptoms.
- Polysomnography (Sleep Study): Cheyne-Stokes respiration often occurs during sleep. Polysomnography, a sleep study, is a valuable diagnostic tool. It monitors various parameters, including oxygen saturation, airflow, and respiratory effort, throughout the night.
- Arterial Blood Gas (ABG) Analysis: Similar to Kussmaul breathing, an ABG test may be performed to assess blood gases and pH balance if Cheyne-Stokes respiration is observed during wakefulness.
- Cardiac Evaluation: Given the association of Cheyne-Stokes respiration with heart failure and other cardiovascular conditions, cardiac evaluation may include an echocardiogram, ECG (electrocardiogram), and other heart-related tests.
- Neurological Assessment: If neurological conditions are suspected as a cause, a neurological evaluation may be necessary, which could include brain imaging (e.g., MRI or CT scan) or other neurodiagnostic tests.
- Management of Underlying Conditions: Treatment often focuses on addressing the underlying cause of Cheyne-Stokes respiration, such as heart failure or stroke. Management plans may include medication adjustments, lifestyle changes, or interventions to improve heart function or neurological status.
Both Kussmaul and Cheyne-Stokes breathing patterns are clinical signs that warrant thorough evaluation and a multidisciplinary approach to determine the underlying conditions and provide appropriate treatment. Healthcare providers will tailor the diagnostic process based on individual patient presentations and clinical suspicion.
Treatment Approaches for Kussmaul and Cheyne-Stokes Breathing
The treatment approaches for Kussmaul and Cheyne-Stokes breathing patterns primarily focus on addressing the underlying causes and associated conditions. Here’s how each abnormal breathing pattern is managed:
Treatment for Kussmaul Breathing:
- Identify and Treat the Underlying Cause:
- The most critical step is to identify and address the root cause of Kussmaul respiration. This often involves diagnostic tests (e.g., arterial blood gas analysis, blood glucose measurement) to determine the specific underlying condition.
- For diabetic ketoacidosis, the primary treatment is insulin therapy to lower blood sugar levels and correct the acidosis.
- If renal failure or metabolic disorders are the cause, treatment may involve addressing the underlying kidney dysfunction or metabolic abnormalities.
- Fluid and Electrolyte Replacement:
- In cases of severe dehydration or electrolyte imbalances, intravenous (IV) fluids and electrolyte supplementation may be necessary to restore balance.
- Correction of Acid-Base Imbalance:
- Treatment aims to correct metabolic acidosis. Depending on the underlying condition, this may involve the administration of bicarbonate or other medications to normalize the body’s pH levels.
- Management of Complications:
- Kussmaul respiration can lead to complications such as electrolyte imbalances, circulatory issues, and organ dysfunction. Management includes addressing these complications as needed.
- Close Monitoring:
- Patients with Kussmaul respiration require close monitoring of vital signs, blood gases, and overall clinical status. Adjustments to treatment plans may be made based on ongoing assessments.
Treatment for Cheyne-Stokes Respiration:
- Address the Underlying Condition:
- The primary approach to managing Cheyne-Stokes respiration is to identify and treat the underlying medical condition causing the abnormal breathing pattern. This often includes:
- For heart failure: Medications to improve heart function, lifestyle modifications, and, in some cases, devices like cardiac resynchronization therapy.
- For stroke: Treatment of the stroke and rehabilitation to improve neurological function.
- For other conditions (e.g., brain tumors, high-altitude hypoxia): Targeted treatments based on the specific diagnosis.
- The primary approach to managing Cheyne-Stokes respiration is to identify and treat the underlying medical condition causing the abnormal breathing pattern. This often includes:
- Positive Airway Pressure Therapy:
- In some cases, continuous positive airway pressure (CPAP) or bilevel positive airway pressure (BiPAP) therapy may be used to improve breathing during sleep and alleviate Cheyne-Stokes respiration. This is often employed when Cheyne-Stokes occurs during sleep as in central sleep apnea.
- Oxygen Therapy:
- Supplemental oxygen therapy may be prescribed to maintain adequate oxygen levels in the blood, particularly for patients with heart failure or conditions causing low oxygen saturation.
- Medications:
- Depending on the underlying cause, medications like diuretics, beta-blockers, or other cardiac medications may be prescribed to manage heart-related issues.
- Lifestyle Modifications:
- Lifestyle changes, including dietary adjustments, weight management, and adherence to prescribed medications, play a significant role in managing Cheyne-Stokes respiration, especially in heart failure cases.
- Regular Follow-Up:
- Patients with Cheyne-Stokes respiration should have regular follow-up appointments with healthcare providers to assess progress, adjust treatments, and monitor any changes in the underlying condition.
The key to effective management of both Kussmaul and Cheyne-Stokes breathing patterns is a comprehensive and individualized approach that addresses the specific underlying causes and the patient’s overall health status. Collaboration among healthcare professionals, including physicians, nurses, respiratory therapists, and specialists, is often necessary to provide optimal care.
Prevention and Risk Reduction
Prevention and risk reduction strategies for Kussmaul and Cheyne-Stokes breathing patterns primarily involve addressing the underlying conditions or risk factors associated with these abnormal respiratory patterns.
Here are some general approaches to prevent or reduce the risk of experiencing these breathing patterns:
Prevention and Risk Reduction for Kussmaul Breathing:
- Diabetes Management:
- If you have diabetes, it’s crucial to manage your blood sugar levels effectively through medication, diet, and regular monitoring. This can help prevent diabetic ketoacidosis, a common cause of Kussmaul respiration.
- Regular Medical Check-Ups:
- Underlying conditions that can lead to Kussmaul respiration, such as kidney disease or metabolic disorders, may be detected early through routine medical check-ups.
- Medication Adherence:
- If you have a medical condition that requires medication (e.g., antiretroviral drugs for HIV), ensure strict adherence to your medication regimen to prevent complications.
- Hydration and Nutrition:
- Maintain proper hydration and balanced nutrition to help prevent metabolic imbalances that can lead to Kussmaul respiration.
- Lifestyle Choices:
- Adopt a healthy lifestyle, including regular exercise and a well-balanced diet, to reduce the risk of developing metabolic disorders.
Prevention and Risk Reduction for Cheyne-Stokes Respiration:
- Manage Cardiovascular Health:
- To reduce the risk of Cheyne-Stokes respiration associated with heart failure or other cardiovascular conditions, manage your heart health through regular exercise, a heart-healthy diet, and adherence to prescribed medications.
- Control Blood Pressure:
- High blood pressure (hypertension) is a risk factor for cardiovascular conditions. Monitoring and controlling blood pressure regularly are excellent ways to lower the chance of it forming.
- Stroke Prevention:
- To lower the risk of Cheyne-Stokes respiration due to stroke, focus on stroke prevention strategies, such as controlling blood pressure, managing diabetes, and quitting smoking.
- Sleep Hygiene:
- Proper sleep hygiene practices can reduce the risk of Cheyne-Stokes respiration during sleep. Maintain a regular sleep schedule and create a comfortable sleep environment.
- Medication Management:
- If you are taking medications that may affect respiration (e.g., opioids), use them only as prescribed and under medical supervision.
- Weight Management:
- Obesity is a risk factor for both heart failure and sleep-related breathing disorders. Maintaining and reaching an ideal weight can greatly decrease the chance of serious illness and disease.
- Quit Smoking and Limit Alcohol Intake:
- Smoking and excessive alcohol consumption can increase the risk of cardiovascular conditions. Quitting smoking and moderating alcohol intake can help reduce these risks.
- Regular Check-Ups:
- Attend regular medical check-ups to monitor your cardiovascular and overall health. Intervention and early diagnosis could help avoid potential complications.
It’s essential to consult with a healthcare provider for personalized advice and to create a prevention plan tailored to your specific risk factors and medical history. Managing underlying conditions and adopting a healthy lifestyle are key components of prevention and risk reduction for both Kussmaul and Cheyne-Stokes breathing patterns.
Conclusion
Kussmaul respiration and Cheyne-Stokes respiration are distinct abnormal breathing patterns, each indicative of underlying medical conditions. Kussmaul respiration involves deep, rapid, and labored breaths, often associated with metabolic acidosis, while Cheyne-Stokes respiration is characterized by a cyclical pattern of alternating breath depth and rate with periods of apnea, typically linked to cardiovascular or neurological issues.
Prompt recognition, accurate diagnosis, and targeted treatment of these patterns are crucial for improving patient outcomes. Prevention and risk reduction strategies involve managing underlying conditions and adopting a healthy lifestyle. Healthcare professionals play a vital role in ensuring proper care and management for individuals exhibiting these respiratory patterns.



